|
1
|
PC4-mediated Ku complex PARylation facilitates NHEJ-dependent DNA damage repair. J Biol Chem 2023; 299:105032. [PMID: 37437887 PMCID: PMC10406618 DOI: 10.1016/j.jbc.2023.105032] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 03/02/2023] [Revised: 07/01/2023] [Accepted: 07/03/2023] [Indexed: 07/14/2023] Open
Abstract
Radiotherapy is one of the mainstay treatments for hepatocellular carcinoma (HCC). However, a substantial number of patients with HCC develop radioresistance and eventually suffer from tumor progression or relapse, which is a major impediment to the use of radiotherapy. Therefore, elucidating the mechanisms underlying radioresistance and identifying novel therapeutic targets to improve patient prognosis are important in HCC management. In this study, using in vitro and in vivo models, laser microirradiation and live cell imaging methods, and coimmunoprecipitation assays, we report that a DNA repair enhancer, human positive cofactor 4 (PC4), promotes nonhomologous end joining-based DNA repair and renders HCC cells resistant to radiation. Mechanistically, PC4 interacts with poly (ADP-ribose) polymerase 1 and directs Ku complex PARylation, resulting in the successful recruitment of the Ku complex to damaged chromatin and increasing the efficiency of nonhomologous end joining repair. Clinically, PC4 is highly expressed in tumor tissues and is correlated with poor prognosis in patients with HCC. Taken together, our data suggest that PC4 is a DNA repair driver that can be targeted to radiosensitize HCC cells.
Collapse
|
|
2
|
Targeting positive cofactor 4 induces autophagic cell death in MYC-expressing diffuse large B-cell lymphoma. Exp Hematol 2023; 119-120:42-57.e4. [PMID: 36642374 DOI: 10.1016/j.exphem.2023.01.001] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 09/30/2022] [Revised: 01/04/2023] [Accepted: 01/05/2023] [Indexed: 01/15/2023]
Abstract
MYC-expressing diffuse large B-cell lymphoma (DLBCL) is one of the refractory lymphomas. Currently, the pathogenesis of MYC-expressing DLBCL is still unclear, and there is a lack of effective therapy. We characterized positive cofactor 4 (PC4) as an upstream regulator of c-Myc, and PC4 is overexpressed in DLBCL and is closely related to clinical staging, prognosis, and c-Myc expression. Furthermore, our in vivo and in vitro studies revealed that PC4 knockdown can induce autophagic cell death and enhance the therapeutic effect of doxorubicin in MYC-expressing DLBCL. Inhibition of c-Myc-mediated aerobic glycolysis and activation of the AMPK/mTOR signaling pathway are responsible for the autophagic cell death induced by PC4 knockdown in MYC-expressing DLBCL. Using dual-luciferase reporter assay and electrophoretic mobility shift assay assays, we also found that PC4 exerts its oncogenic functions by directly binding to c-Myc promoters. To sum up, our study provides novel insights into the functions and mechanisms of PC4 in MYC-expressing DLBCL and suggests that PC4 may be a promising therapeutic target for MYC-expressing DLBCL.
Collapse
|
|
3
|
Identification of a three-gene prognostic signature for radioresistant esophageal squamous cell carcinoma. World J Clin Oncol 2023; 14:13-26. [PMID: 36699628 PMCID: PMC9850665 DOI: 10.5306/wjco.v14.i1.13] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Journal Information] [Submit a Manuscript] [Subscribe] [Scholar Register] [Received: 07/25/2022] [Revised: 10/25/2022] [Accepted: 12/06/2022] [Indexed: 01/10/2023] Open
Abstract
BACKGROUND Esophageal squamous cell carcinoma (ESCC) is causing a high mortality rate due to the lack of efficient early prognosis markers and suitable therapeutic regimens. The prognostic role of genes responsible for the acquisition of radioresistance in ESCC has not been fully elucidated.
AIM To establish a prognostic model by studying gene expression patterns pertinent to radioresistance in ESCC patients.
METHODS Datasets were obtained from the Gene Expression Omnibus and The Cancer Genome Atlas databases. The edgeR, a Bioconductor package, was used to analyze mRNA expression between different groups. We screened genes specifically responsible for radioresistance to estimate overall survival. Pearson correlation analysis was performed to confirm whether the expression of those genes correlated with each other. Genes contributing to radioresistance and overall survival were assessed by the multivariate Cox regression model through the calculation of βi and risk score using the following formula: 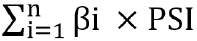 . .
RESULTS We identified three prognostic mRNAs (cathepsin S [CTSS], cluster of differentiation 180 [CD180], and SLP adapter and CSK-interacting membrane protein [SCIMP]) indicative of radioresistance. The expression of the three identified mRNAs was related to each other (r > 0.70 and P < 0.05). As to 1-year and 3-year overall survival prediction, the area under the time-dependent receiver operating characteristic curve of the signature consisting of the three mRNAs was 0.716 and 0.841, respectively. When stratifying patients based on the risk score derived from the signature, the high-risk group exhibited a higher death risk and shorter survival time than the low-risk group (P < 0.0001). Overall survival of the low-risk patients was significantly better than that of the high-risk patients (P = 0.018).
CONCLUSION We have developed a novel three-gene prognostic signature consisting of CTSS, CD180, and SCIMO for ESCC, which may facilitate the prediction of early prognosis of this malignancy.
Collapse
|
|
4
|
Cancer stem cells in esophageal squamous cell carcinoma. Pathol Res Pract 2022; 237:154043. [DOI: 10.1016/j.prp.2022.154043] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Track Full Text] [Journal Information] [Submit a Manuscript] [Subscribe] [Scholar Register] [Received: 06/21/2022] [Revised: 07/21/2022] [Accepted: 07/26/2022] [Indexed: 02/07/2023]
|
|
5
|
Positive Cofactor 4 as a Potential Radiation Biodosimeter for Early Assessment. Dose Response 2022; 20:15593258221081317. [PMID: 35221823 PMCID: PMC8874181 DOI: 10.1177/15593258221081317] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Indexed: 11/17/2022]
Abstract
During a major radiation event, a large number of people need to be rapidly assessed for radiation damage to ensure effective medical treatment and efficient use of medical resources. However, current techniques cannot meet the requirement of rapid detection of large quantities of samples in an emergency. It is essential to develop rapid and accurate radiation biodosimeters in peripheral blood. Here, we identified radiation sensitive genes in mice by RNA sequencing and evaluated their utility as radiation biodosimeters in human cell lines. Mice were subjected to gamma-irradiation with different doses (0–8 Gy, .85 Gy/min), and the tail venous blood was analyzed by RNA sequencing. We have identified 5 genes with significantly differential expression after radiation exposure. We found that positive cofactor 4(PC4) had well correlation with radiation dose in human lymphoblastoid cell line after irradiation. The relative expression of PC4 gene showed a good linear correlation with the radiation dose after 1–5 Gy irradiation (.85 Gy/min). PC4 gene can be rapidly recruited to the DNA damage sites faster than γ-H2AX after radiation in immunofluorescence detection. In conclusion, PC4 may be represented as new radiation biological dosimeter for early assessment.
Collapse
|
|
6
|
MicroRNA-29b regulates the radiosensitivity of esophageal squamous cell carcinoma by regulating the BTG2-mediated cell cycle. Strahlenther Onkol 2021; 197:829-835. [PMID: 34232332 DOI: 10.1007/s00066-021-01790-5] [Citation(s) in RCA: 1] [Impact Index Per Article: 0.3] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/04/2021] [Accepted: 04/20/2021] [Indexed: 01/13/2023]
Abstract
BACKGROUND Many patients with esophageal squamous cell carcinoma (ESCC) are inoperable due to old age or advanced stage; thus, radio- and chemotherapy are considered the standard treatments for these patients. However, due to the radiation resistance of tumor cells that may arise during radiotherapy, results are still not satisfactory. The authors' previous studies found that microRNA can affect radiosensitivity, and further microRNA research was conducted to improve the radiosensitivity of ESCC. METHODS Cells were treated with silent miR-29b (si-miR-29b). Thereafter,proliferation, colony formation, cell cycle, and apoptosis were determined. The luciferase reporting assay was used to confirm the direct interaction between miR-29b and BTG2. Serum samples and clinical follow-up data of 75 elderly or advanced ESCC patients who could not tolerate surgery were collected. RESULTS The expression level of miR-29 in ESCC serum was closely correlated to radiosensitivity (χ2 =8.36, p < 0.05) and correlated with overall survival (OS; hazard ratio [HR] 0.47, 95% confidence interval [CI] 0.24-0.90). Function assays demonstrated that the number of cell clones increased after radiometry radiation, and the cell cycle was blocked in the G0/G1 phase (from 37.2 to 56.9%) in the si-miR-29b transfection group. Expression of BTG2 was upregulated and expression of cyclin D1 was downregulated (p < 0.05). Transfection of si-BTG2 can reverse this result and restore the expression level of cyclin D1 (p < 0.05). The target gene BTG2 of miR-29b was predicted using a bioinformatics tool and confirmed by dual-luciferase reporter assay. CONCLUSION Silencing of miR-29b in ESCC cells can increase expression of BTG2 and decrease the level of intracellular cyclin D1, resulting in cell cycle arrest and accumulation in the G0/G1 phase. Because G0/G1-phase cells are insensitive to radiotherapy, the sensitivity of radiotherapy is reduced.
Collapse
|
|
7
|
FMS-Related Tyrosine Kinase 3 Ligand Promotes Radioresistance in Esophageal Squamous Cell Carcinoma. Front Pharmacol 2021; 12:659735. [PMID: 34040525 PMCID: PMC8141745 DOI: 10.3389/fphar.2021.659735] [Citation(s) in RCA: 7] [Impact Index Per Article: 2.3] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/28/2021] [Accepted: 04/26/2021] [Indexed: 11/23/2022] Open
Abstract
Aim: The FMS-related tyrosine kinase 3 ligand (FL) has an important role in regulating FMS-related tyrosine kinase 3 (Flt-3) activity. Serum FL levels are markedly increased among patients with hematopoietic disease. However, its role in radiation treatment remains unclear. In this study, we investigated the effects of FL on radiotherapy for esophageal squamous cell carcinoma (ESCC). Methods: KYSE150 and KYSE450 cells were stimulated with FL (200 ng/ml). mRNA expression was analyzed using qRT-PCR. Cell viability was checked using CCK-8 assay kits. Proliferation was determined using the EdU assay. Radiosensitivity was detected through a colony-forming assay. Flow cytometry was used to evaluate cell apoptosis. The number of γH2AX foci was verified using an immunofluorescence assay. The change in relative proteins was determined by western blot analysis. The growth of transplanted tumors was demonstrated in nude mice. Results: Our results showed that FL increased the radiation resistance of ESCC cells by promoting clone formation, increasing EdU incorporation, enhancing DNA damage repair, and inhibiting apoptosis. Moreover, the Flt-3 receptor expression significantly increased in ESCC cells after radiation, which may have been an important factor in their radioresistance. Conclusion: Our results suggest that FL increases the radioresistance of esophageal cancer cells and that FL-Flt-3 could be a potential target for enhancing radiosensitivity in ESCC.
Collapse
|
|
8
|
The mechanisms and reversal strategies of tumor radioresistance in esophageal squamous cell carcinoma. J Cancer Res Clin Oncol 2021; 147:1275-1286. [PMID: 33687564 DOI: 10.1007/s00432-020-03493-3] [Citation(s) in RCA: 22] [Impact Index Per Article: 7.3] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 11/03/2020] [Accepted: 12/02/2020] [Indexed: 01/16/2023]
Abstract
Esophageal squamous cell carcinoma (ESCC) is one of most lethal malignancies with high aggressive potential in the world. Radiotherapy is used as one curative treatment modality for ESCC patients. Due to radioresistance, the 5-year survival rates of patients after radiotherapy is less than 20%. Tumor radioresistance is very complex and heterogeneous. Cancer-associated fibroblasts (CAFs), as one major component of tumor microenvironment (TME), play critical roles in regulating tumor radioresponse through multiple mechanisms and are increasingly considered as important anti-cancer targets. Cancer stemness, which renders cancer cells to be extremely resistant to conventional therapies, is involved in ESCC radioresistance due to the activation of Wnt/β-catenin, Notch, Hedgehog and Hippo (HH) pathways, or the induction of epithelial-mesenchymal transition (EMT), hypoxia and autophagy. Non-protein-coding RNAs (ncRNAs), which account for more than 90% of the genome, are involved in esophageal cancer initiation and progression through regulating the activation or inactivation of downstream signaling pathways and the expressions of target genes. Herein, we mainly reviewed the role of CAFs, cancer stemness, non-coding RNAs as well as others in the development of radioresistance and clarify the involved mechanisms. Furthermore, we summarized the potential strategies which were reported to reverse radioresistance in ESCC. Together, this review gives a systematic coverage of radioresistance mechanisms and reversal strategies and contributes to better understanding of tumor radioresistance for the exploitation of novel intervention strategies in ESCC.
Collapse
|
|
9
|
Knockdown of PC4 increases chemosensitivity of Oxaliplatin in triple negative breast cancer by suppressing mTOR pathway. Biochem Biophys Res Commun 2021; 544:65-72. [PMID: 33524870 DOI: 10.1016/j.bbrc.2021.01.029] [Citation(s) in RCA: 1] [Impact Index Per Article: 0.3] [Reference Citation Analysis] [Abstract] [Key Words] [Journal Information] [Subscribe] [Scholar Register] [Received: 12/26/2020] [Accepted: 01/11/2021] [Indexed: 11/29/2022]
Abstract
As a multifunctional nuclear protein, the human positive cofactor 4 (PC4) is highly expressed in various tumors including breast cancer and has potential roles in cancer development and progression. However, the functional signatures and molecular mechanisms of PC4 in triple negative breast cancer (TNBC) progression and chemotherapeutic response are still unknown. In this study, we found that PC4 is significantly upregulated in TNBC cells compared with non-TNBC cells, implying its potential role in TNBC. Then, in vivo and in vitro studies revealed that knockdown of PC4 increased chemosensitivity of Oxaliplation (Oxa) in TNBC by suppressing mTOR pathway. Therefore, our findings demonstrated the signatures and molecular mechanisms of PC4 in TNBC chemotherapeutic response, and indicated that PC4 might be a promising therapeutic target for TNBC.
Collapse
|
|
10
|
Inhibitors of DNA double-strand break repair at the crossroads of cancer therapy and genome editing. Biochem Pharmacol 2020; 182:114195. [DOI: 10.1016/j.bcp.2020.114195] [Citation(s) in RCA: 6] [Impact Index Per Article: 1.5] [Reference Citation Analysis] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 06/01/2020] [Revised: 08/03/2020] [Accepted: 08/10/2020] [Indexed: 12/17/2022]
|
|
11
|
Human Positive Coactivator 4 Affects the Progression and Prognosis of Pancreatic Ductal Adenocarcinoma via the mTOR/P70s6k Signaling Pathway. Onco Targets Ther 2020; 13:12213-12223. [PMID: 33273827 PMCID: PMC7705283 DOI: 10.2147/ott.s284219] [Citation(s) in RCA: 2] [Impact Index Per Article: 0.5] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 09/30/2020] [Accepted: 11/17/2020] [Indexed: 12/13/2022] Open
Abstract
Introduction Pancreatic cancer is one of the deadliest cancers in the world, and pancreatic ductal adenocarcinoma (PDAC) accounts for 90% of all cases. Human positive coactivator 4 (PC4) is a transcriptional coactivator that has been associated with the development and progression of several tumors. However, no studies investigated the potential role of PC4 in PDAC. Methods We investigated PC4 expression in 81 PDAC tissue samples using immunohistochemistry and studied the impact of PC4 expression and the molecular mechanisms of this altered expression on PDAC tumorigenesis and proliferation both in vitro and in vivo. Results PC4 overexpression was correlated with a poor outcome in PDAC patients. The RNAi-mediated knockdown of PC4 expression in CFPAC-1 and AsPC-1 cell lines reduced cell proliferation and tumor growth. The loss of PC4 in PDAC inhibits cell growth by inducing cell cycle arrest at the G1/S transition and suppressing the mTOR/p70s6k pathway. Discussion/Conclusion Our findings reveal for the first time that PC4 exerts oncogenic functions by activating mTOR/p70s6k signaling pathway-mediated cell proliferation, implying that PC4 is a promising therapeutic target for PDAC.
Collapse
|
|
12
|
Value of long non-coding RNA Rpph1 in esophageal cancer and its effect on cancer cell sensitivity to radiotherapy. World J Gastroenterol 2020; 26:1775-1791. [PMID: 32351293 PMCID: PMC7183868 DOI: 10.3748/wjg.v26.i15.1775] [Citation(s) in RCA: 6] [Impact Index Per Article: 1.5] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Download PDF] [Journal Information] [Submit a Manuscript] [Subscribe] [Scholar Register] [Received: 12/11/2019] [Revised: 01/23/2020] [Accepted: 03/19/2020] [Indexed: 02/06/2023] Open
Abstract
BACKGROUND Esophageal cancer is a common digestive tract tumor that is generally treated with radiotherapy. Poor responses to radiotherapy in most patients generally result in local radiotherapy failure, so it is essential to find new radiosensitizers that can enhance the response of cancer cells to radiotherapy and improve the survival of esophageal cancer patients with radiation resistance. The long non-coding RNA (lncRNA) Rpph1 is highly expressed in human gastric cancer tissues, and represses breast cancer cell proliferation and tumorigenesis. However, the expression of lncRNA Rpph1 in esophageal cancer and its relationship with radio-sensitivity has not been studied.
AIM To explore the value of lncRNA Rpph1 in esophageal cancer and its effect on cancer cell sensitivity to radiotherapy.
METHODS Eighty-three patients with esophageal cancer admitted to Qilu Hospital of Shandong University and 90 healthy participants who received physical examinations were collected as research participants. The expression of Rpph1 was determined by qRT-PCR. siRNA-NC and siRNA-Rpph1 were transfected into esophageal cancer cell lines, and cells without transfection were designated as the blank control group. Cell survival was tested by colony formation assays, and the levels of proteins related to apoptosis and epithelial-mesenchymal transitions were determined by Western blot assays. Cell proliferation was assessed by MTT assays, cell apoptosis by flow cytometry, and cell migration by wound-healing assays. Changes in cell cycle distribution were monitored.
RESULTS Rpph1 was highly expressed in esophageal carcinoma, making it a promising marker for the diagnosis of esophageal cancer. Rpph1 could also be used to distinguish different short-term responses, T stages, N stages, and clinical stages of esophageal cancer patients. The results of 3-year overall survival favored patients with lower Rpph1 expression over patients with higher Rpph1 expression (P < 0.05). In vitro and in vivo experiments showed that silencing Rpph1 expression led to higher sensitivity of esophageal cancer cells to radiotherapy, stronger apoptosis in esophageal cancer cells induced by radiotherapy, higher expression of Bax and caspase-3, and lower expression of Bcl-2 (Bax, caspase-3, and Bcl-2 are apoptosis-related proteins). Additionally, silencing Rpph1 attenuated radiation-induced G2/M phase arrest, and significantly inhibited the expression of proteins involved in cell proliferation, migration, and epithelial-mesenchymal transition regulation in esophageal cancer cells.
CONCLUSION Rpph1 is highly expressed in esophageal cancer. Silencing Rpph1 expression can promote cell apoptosis, inhibit cell proliferation and migration, and increase radio-sensitivity.
Collapse
|
|
13
|
Efficacy of a small molecule inhibitor of the transcriptional cofactor PC4 in prevention and treatment of non-small cell lung cancer. PLoS One 2020; 15:e0230670. [PMID: 32231397 PMCID: PMC7108703 DOI: 10.1371/journal.pone.0230670] [Citation(s) in RCA: 2] [Impact Index Per Article: 0.5] [Reference Citation Analysis] [Abstract] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 09/03/2019] [Accepted: 03/05/2020] [Indexed: 12/19/2022] Open
Abstract
The human positive coactivator 4 (PC4) was originally identified as a multi-functional cofactor capable of mediating transcription activation by diverse gene- and tissue-specific activators. Recent studies suggest that PC4 might also function as a novel cancer biomarker and therapeutic target for different types of cancers. siRNA knockdown studies indicated that down-regulation of PC4 expression could inhibit tumorigeneicity of A549 non-small cell lung cancer tumor model in nude mice. Here we show that AG-1031, a small molecule identified by high throughput screening, can inhibit the double-stranded DNA binding activity of PC4, more effectively than its single-stranded DNA binding activity. AG-1031 also specifically inhibited PC4-dependent transcriptional activation in vitro using purified transcription factors. AG-1031 inhibited proliferation of several cultured cell lines derived from non-small cell lung cancers (NSCLC) and growth of tumors that formed from A549 cell xenografts in immuno-compromised mice. Moreover, pre-injection of AG-1031 in these mice not only reduced tumor size, but also prevented tumor formation in 20% of the animals. AG-1031 treated A549 cells and tumors from AG-1031 treated animals showed a significant decrease in the levels of both PC4 and VEGFC, a key mediator of angiogenesis in cancer. On the other hand, all tested mice remained constant weight during animal trials. These results demonstrated that AG-1031 could be a potential therapy for PC4-positive NSCLC.
Collapse
|
|
14
|
NVP-BSK805, an Inhibitor of JAK2 Kinase, Significantly Enhances the Radiosensitivity of Esophageal Squamous Cell Carcinoma in vitro and in vivo. DRUG DESIGN DEVELOPMENT AND THERAPY 2020; 14:745-755. [PMID: 32158193 PMCID: PMC7047839 DOI: 10.2147/dddt.s203048] [Citation(s) in RCA: 2] [Impact Index Per Article: 0.5] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Subscribe] [Scholar Register] [Received: 01/27/2019] [Accepted: 01/10/2020] [Indexed: 01/22/2023]
Abstract
Purpose Radiotherapy is one major curative treatment modality for esophageal squamous cell carcinoma (ESCC) patients. This study aimed to find out small-molecular kinase inhibitors, which can significantly enhance the radiosensitivity of ESCC in vitro and in vivo. Materials and Methods Ninety-three kinase inhibitors were tested for their radiosensitizing effect in ESCC cells through high-content screening. The radiosensitizing effect of kinase inhibitors was investigated in vitro by detection of DNA double-strand breaks (DSBs) and clonogenic survival assay. By the establishment of xenograft tumor models in BALB/c nude mice, the radiosensitizing effect of kinase inhibitors was investigated in vivo. Results Among the 93 kinase inhibitors tested, we found NVP-BSK805, an inhibitor of JAK2 kinase, significantly radiosensitized ESCC cells through enhancing DSBs, inhibiting DNA damage repair and arresting cell cycle in G2/M or G0/G1 phase. After treatment with NVP-BSK805, ESCC cells showed decreased clonogenic survival and delayed tumor growth in vivo. JAK2 kinase was highly expressed in tumor tissues of ESCC patients, while rarely expressed in matched normal esophageal epithelial tissues. Survival analysis revealed JAK2 kinase as a prognostic factor of ESCC patients treated with chemoradiotherapy. Conclusion Our study discovered JAK2 kinase as an attractive target to enhance the radiosensitivity of ESCC cells in vitro and in vivo.
Collapse
|
|
15
|
Chromatin protein PC4 is downregulated in breast cancer to promote disease progression: Implications of miR-29a. Oncotarget 2019; 10:6855-6869. [PMID: 31839879 PMCID: PMC6901337 DOI: 10.18632/oncotarget.27325] [Citation(s) in RCA: 1] [Impact Index Per Article: 0.2] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 05/15/2019] [Accepted: 10/19/2019] [Indexed: 02/05/2023] Open
Abstract
The human transcriptional coactivator PC4 has numerous roles to play in the cell. Other than its transcriptional coactivation function, it facilitates chromatin organization, DNA damage repair, viral DNA replication, etc. Although it was found to be an essential protein in vivo, the importance of this multifunctional protein in the regulation of different cellular pathways has not been investigated in details, particularly in oncogenesis. In this study, PC4 downregulation was observed in a significant proportion of mammary tissues obtained from Breast cancer patient samples as well as in a subset of highly invasive and metastatic Breast cancer patient-derived cell lines. We have identified a miRNA, miR-29a which potentially reduce the expression of PC4 both in RNA and protein level. This miR-29a was found to be indeed overexpressed in a substantial number of Breast cancer patient samples and cell lines as well, suggesting one of the key mechanisms of PC4 downregulation. Stable Knockdown of PC4 in MCF7 cells induced its migratory as well as invasive properties. Furthermore, in an orthotopic breast cancer mice model system; we have shown that reduced expression of PC4 enhances the tumorigenic potential substantially. Absence of PC4 led to the upregulation of several genes involved in Epithelial to Mesenchymal Transition (EMT), indicating the possible mechanism of uniform tumour progression in the orthotropic mice. Collectively these data establish the role of PC4 in tumour suppression.
Collapse
|
|
16
|
An NIR‐Fluorophore‐Based Inhibitor of SOD1 Induces Apoptosis by Targeting Transcription Cofactor PC4. ADVANCED THERAPEUTICS 2019. [DOI: 10.1002/adtp.201800148] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Indexed: 11/06/2022]
|
|
17
|
Transcriptional positive cofactor 4 promotes breast cancer proliferation and metastasis through c-Myc mediated Warburg effect. Cell Commun Signal 2019; 17:36. [PMID: 30992017 PMCID: PMC6469038 DOI: 10.1186/s12964-019-0348-0] [Citation(s) in RCA: 20] [Impact Index Per Article: 4.0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/10/2019] [Accepted: 04/03/2019] [Indexed: 12/24/2022] Open
Abstract
Background The human positive cofactor 4 (PC4) is initially identified as a transcriptional cofactor and has an important role in embryonic development and malignant transformation. However, the clinical significance and the molecular mechanisms of PC4 in breast cancer development and progression are still unknown. Methods We investigated PC4 expression in 114 cases of primary breast cancer and matched normal breast tissue specimens, and studied the impact of PC4 expression as well as the molecular mechanisms of this altered expression on breast cancer growth and metastasis both in vitro and in vivo. Results PC4 was significantly upregulated in breast cancer and high PC4 expression was positively correlated with metastasis and poor prognosis of patients. Gene set enrichment analysis (GSEA) demonstrated that the gene sets of cell proliferation and Epithelial-Mesenchymal Transition (EMT) were positively correlated with elevated PC4 expression. Consistently, loss of PC4 markedly inhibited the growth and metastasis of breast cancer both in vitro and in vivo. Mechanistically, PC4 exerted its oncogenic functions by directly binding to c-Myc promoters and inducing Warburg effect. Conclusions Our study reveals for the first time that PC4 promotes breast cancer progression by directly regulating c-Myc transcription to promote Warburg effect, implying a novel therapeutic target for breast cancer. Electronic supplementary material The online version of this article (10.1186/s12964-019-0348-0) contains supplementary material, which is available to authorized users.
Collapse
|
|
18
|
The human positive cofactor 4 promotes androgen-independent prostate cancer development and progression through HIF-1α/β-catenin pathway. Am J Cancer Res 2019; 9:682-698. [PMID: 31105996 PMCID: PMC6511634] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [Journal Information] [Subscribe] [Scholar Register] [Received: 03/01/2019] [Accepted: 03/15/2019] [Indexed: 06/09/2023] Open
Abstract
Androgen-dependent prostate cancer (ADPC) eventually progresses to androgen-independent prostate cancer (AIPC), that has a poor prognosis owing to its unclear mechanism and lack of effective therapeutic targets. The human positive cofactor 4 (PC4) is a transcriptional cofactor, and plays a potential role in cancer development. However, the significance and mechanism of PC4 in AIPC progression are unclear. By analyzing the clinical data, we find that PC4 is overexpressed in prostate cancer and closely correlated with the progression, metastasis and prognosis of patients. Additionally, PC4 is significantly upregulated in AIPC cells compared with ADPC cells, implying its importance in the development and progression of AIPC. Then, in vivo and in vitro studies reveal that loss of PC4 inhibits cell growth by suppressing c-Myc/P21 pathway and inducing cell cycle arrest at G1/S phase transition in AIPC. PC4 knockdown also attenuates EMT-mediated metastasis in AIPC. Moreover, for the first time, we find that PC4 exerts its oncogenic functions by promoting the expression of HIF-1α and activating β-catenin signaling. Therefore, our findings determine the signatures and molecular mechanisms of PC4 in AIPC, and indicate that PC4 might be a promising therapeutic target for AIPC.
Collapse
|
|
19
|
Silencing of XRCC4 increases radiosensitivity of triple-negative breast cancer cells. Biosci Rep 2019; 39:BSR20180893. [PMID: 30842344 PMCID: PMC6423307 DOI: 10.1042/bsr20180893] [Citation(s) in RCA: 12] [Impact Index Per Article: 2.4] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 06/05/2018] [Revised: 02/13/2019] [Accepted: 03/05/2019] [Indexed: 01/04/2023] Open
Abstract
Background: Radiotherapy is an important locoregional treatment, and its effect on triple-negative breast cancer (TNBC) needs to be enhanced. The aim of the present study was to investigate the potential effects of XRCC4 on radiosensitivity of TNBC. Methods: The RNAi technique was implemented to establish the TNBC stable cell line with XRCC4 knockdown. MTT assay was used to detect the effect of XRCC4 knockdown on cell proliferation. Western blot and immunohistochemistry assays were employed to identify protein expression. Colony assay was performed to detect the effect of XRCC4 knockdown on the colony formation ability of TNBC cells with radiation treatment. Comet assay was conducted to evaluate the influence of XRCC4 silencing on DNA repair activity in ionizing radiation. In addition, we performed a survival analysis based on data in TCGA database. Results: XRCC4 knockdown by lentivirus-mediated shRNA had no significant effect on proliferation of TNBC cells. Knockdown of XRCC4 could substantially increase the sensitivity of TNBC cells to ionizing radiation. The DNA damage level was detected to be increased in the XRCC4 knockdown group, indicating there was a significant repair delay in the XRCC4-deleted cells. Clinical sample analysis exhibited that there were various XRCC4 expression in different patients with TNBC. Moreover, survival analysis showed that high expression of XRCC4 was significantly associated with poor progression-free survival after radiotherapy in TNBC patients. Conclusion: Our findings suggest that XRCC4 knockdown sensitizes TNBC cells to ionizing radiation, and could be considered as a novel predictor of radiosensitivity and a promising target for TNBC.
Collapse
|
|
20
|
Therapeutic effect of dental pulp stem cell transplantation on a rat model of radioactivity-induced esophageal injury. Cell Death Dis 2018; 9:738. [PMID: 29970894 PMCID: PMC6030227 DOI: 10.1038/s41419-018-0753-0] [Citation(s) in RCA: 17] [Impact Index Per Article: 2.8] [Reference Citation Analysis] [Abstract] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/29/2018] [Revised: 05/09/2018] [Accepted: 05/22/2018] [Indexed: 01/14/2023]
Abstract
Dental pulp stem cell (DPSC) transplantation has been demonstrated to promote the regeneration and repair of tissues and organs and is a potentially effective treatment for radioactive esophageal injury. In this study, to explore the therapeutic effects of DPSCs on acute radiation-induced esophageal injury, DPSCs were cultured and transplanted into rats with acute radioactive esophageal injuries induced by radioactive 125I seeds in vivo. In the injured esophagus, PKH26-labeled DPSCs co-localized with PCNA, CK14, CD71, and integrin α6, and the expression levels of these four makers of esophageal stem cells were significantly increased. After DPSC transplantation, the injured esophagus exhibited a greater thickness. In addition, the esophageal function and inflammation recovered faster. The results demonstrated that transplanted DPSCs, which trans-differentiated into esophageal stem cells in vivo, could repair the damaged esophageal tissue.
Collapse
|
|
21
|
Abstract
Positive cofactor 4 (PC4) participates in DNA damage repair and involved in nonhomologous end joining (NHEJ). Our previous results demonstrated that knockdown of PC4 downregulated the expression of XRCC4-like factor (XLF) in esophageal squamous cell carcinoma. However, the mechanism how PC4 regulates the expression of XLF remains unclear. Here, we found that knockdown of PC4 increased radiosensitivity of non-small cell lung cancer (NSCLC) both in vivo and in vitro. Furthermore, we found that PC4 knockdown downregulated the expression of XLF, whereas recovering XLF expression restored radioresistance in the PC4-knockdown NSCLC cells. In addition, PC4 knockdown inhibited XLF expression by transcriptionally suppressing of XLF. Moreover, PC4 expression correlated with radiosensitivity and was an independent prognostic factor of progression-free survival (PFS) in patients with NSCLC. These findings suggest that PC4 could be used as a promising therapeutic target for NSCLC.
Collapse
|
|
22
|
CAF-secreted CXCL1 conferred radioresistance by regulating DNA damage response in a ROS-dependent manner in esophageal squamous cell carcinoma. Cell Death Dis 2017; 8:e2790. [PMID: 28518141 PMCID: PMC5520705 DOI: 10.1038/cddis.2017.180] [Citation(s) in RCA: 79] [Impact Index Per Article: 11.3] [Reference Citation Analysis] [Abstract] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 10/15/2016] [Revised: 03/02/2017] [Accepted: 03/03/2017] [Indexed: 12/17/2022]
Abstract
Five-year survival rate of esophageal squamous cell carcinoma (ESCC) patients treated with radiotherapy is <20%. Our study aimed to investigate whether cancer-associated fibroblasts (CAFs), one major component of tumor microenvironment, were involved in tumor radioresistance in ESCC. By use of human chemokine/cytokine array, human chemokine CXCL1 was found to be highly expressed in CAFs compared with that in matched normal fibroblasts. Inhibition of CXCL1 expression in CAFs significantly reversed CAF-conferred radioresistance in vitro and in vivo. CAF-secreted CXCL1 inhibited the expression of reactive oxygen species (ROS)-scavenging enzyme superoxide dismutase 1, leading to increased ROS accumulation following radiation, by which DNA damage repair was enhanced and the radioresistance was mediated. CAF-secreted CXCL1 mediated the radioresistance also by activation of Mek/Erk pathway. The cross talk of CAFs and ESCC cells induced CXCL1 expression in an autocrine/paracrine signaling loop, which further enhanced tumor radioresistance. Together, our study highlighted CAF-secreted CXCL1 as an attractive target to reverse tumor radioresistance and can be used as an independent prognostic factor of ESCC patients treated with chemoradiotherapy.
Collapse
|
|
23
|
A biochemical and biophysical model of G-quadruplex DNA recognition by positive coactivator of transcription 4. J Biol Chem 2017; 292:9567-9582. [PMID: 28416612 DOI: 10.1074/jbc.m117.776211] [Citation(s) in RCA: 6] [Impact Index Per Article: 0.9] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/18/2017] [Revised: 04/14/2017] [Indexed: 12/22/2022] Open
Abstract
DNA sequences that are guanine-rich have received considerable attention because of their potential to fold into a secondary, four-stranded DNA structure termed G-quadruplex (G4), which has been implicated in genomic instability and some human diseases. We have previously identified positive coactivator of transcription (PC4), a single-stranded DNA (ssDNA)-binding protein, as a novel G4 interactor. Here, to expand on these previous observations, we biochemically and biophysically characterized the interaction between PC4 and G4DNA. PC4 can bind alternative G4DNA topologies with a low nanomolar Kd value of ∼2 nm, similar to that observed for ssDNA. In consideration of the different structural features between G4DNA and ssDNA, these binding data indicated that PC4 can interact with G4DNA in a manner distinct from ssDNA. The stoichiometry of the PC4-G4 complex was 1:1 for PC4 dimer:G4 substrate. PC4 did not enhance the rate of folding of G4DNA, and formation of the PC4-G4DNA complex did not result in unfolding of the G4DNA structure. We assembled a G4DNA structure flanked by duplex DNA. We find that PC4 can interact with this G4DNA, as well as the complementary C-rich strand. Molecular docking simulations and DNA footprinting experiments suggest a model where a PC4 dimer accommodates the DNA with one monomer on the G4 strand and the second monomer bound to the C-rich strand. Collectively, these data provide a novel mode of PC4 binding to a DNA secondary structure that remains within the framework of the model for binding to ssDNA. Additionally, consideration of the PC4-G4DNA interaction could provide insight into the biological functions of PC4, which remain incompletely understood.
Collapse
|
|
24
|
The mechanisms of radioresistance in esophageal squamous cell carcinoma and current strategies in radiosensitivity. J Thorac Dis 2017; 9:849-859. [PMID: 28449496 PMCID: PMC5394057 DOI: 10.21037/jtd.2017.03.23] [Citation(s) in RCA: 51] [Impact Index Per Article: 7.3] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 10/07/2016] [Accepted: 01/19/2017] [Indexed: 12/21/2022]
Abstract
Esophageal cancer is the eighth most common cancer and the sixth leading cause of cancer-related death worldwide. Surgery is the primary form of treatment, but the survival is poor, especially for patients with locally advanced esophageal cancer. Radiotherapy has been a critical treatment option that may be combined with chemotherapy in patients with unresectable esophageal cancer. However, resistance to chemoradiotherapy might result in treatment failures and cancer relapse. This review will mainly focus on the possible cellular mechanisms and tumor-associated microenvironmental (TAM) factors that result in radioresistance in patients with esophageal cancer. In addition, current strategies to increase radiosensitivity, including targeted therapy and the use of radiosensitive biomarkers in clinical treatment, are discussed in this review.
Collapse
|
|
25
|
Abstract
This study aims to explore the radiosensitivity of sunitinib on esophageal cancer cell lines. For in vitro studies, human esophageal squamous cell carcinoma (ESCC) cell lines were treated with sunitinib 24 hours before irradiation. ESCC cell lines were treated with sunitinib with or without radiation. Cell proliferation was detected by Cell Counting Kit 8 assay. Radiosensitization was evaluated by clonogenic survival assay. Cell apoptosis and cell cycle analysis were detected by flow cytometry. Deoxyribonucleic acid (DNA) double-strand breaks were performed by immunocytofluorescence analysis. Western blot analysis was used to determine the effect of sunitinib on radiation induced signal transduction. Sunitinib potently sensitized ESCC cells to radiation with a sensitization enhancement ratio of 1.13-1.72. Furthermore, sunitinib increased radiation induced DNA double-strand breaks, promoted the apoptosis of ESCC cells and induced the G2/M arrest. Radiosensitization was accompanied with enhanced apoptosis and regulated by the intrinsic pathway of apoptosis. Sunitinib sensitized ESCC cells to the cytotoxic effects of radiation. This compound is promising for future clinical trials with chemoradiation in esophageal cancer.
Collapse
|
|
26
|
Positive Cofactor 4 (PC4) is critical for DNA repair pathway re-routing in DT40 cells. Sci Rep 2016; 6:28890. [PMID: 27374870 PMCID: PMC4931448 DOI: 10.1038/srep28890] [Citation(s) in RCA: 8] [Impact Index Per Article: 1.0] [Reference Citation Analysis] [Abstract] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 02/09/2016] [Accepted: 06/09/2016] [Indexed: 01/06/2023] Open
Abstract
PC4 is an abundant single-strand DNA binding protein that has been implicated in transcription and DNA repair. Here, we show that PC4 is involved in the cellular DNA damage response. To elucidate the role, we used the DT40 chicken B cell model, which produces clustered DNA lesions at Ig loci via the action of activation-induced deaminase. Our results help resolve key aspects of immunoglobulin diversification and suggest an essential role of PC4 in repair pathway choice. We show that PC4 ablation in gene conversion (GC)-active cells significantly disrupts GC but has little to no effect on targeted homologous recombination. In agreement, the global double-strand break repair response, as measured by γH2AX foci analysis, is unperturbed 16 hours post irradiation. In cells with the pseudo-genes removed (GC inactive), PC4 ablation reduced the overall mutation rate while simultaneously increasing the transversion mutation ratio. By tagging the N-terminus of PC4, gene conversion and somatic hypermutation are all but abolished even when native non-tagged PC4 is present, indicating a dominant negative effect. Our data point to a very early and deterministic role for PC4 in DNA repair pathway re-routing.
Collapse
|
|
27
|
MicroRNA-101 regulated transcriptional modulator SUB1 plays a role in prostate cancer. Oncogene 2016; 35:6330-6340. [PMID: 27270442 PMCID: PMC5140777 DOI: 10.1038/onc.2016.164] [Citation(s) in RCA: 47] [Impact Index Per Article: 5.9] [Reference Citation Analysis] [Abstract] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/11/2016] [Revised: 03/30/2016] [Accepted: 04/06/2016] [Indexed: 12/20/2022]
Abstract
MicroRNA-101, a tumor suppressor microRNA (miR), is often downregulated in cancer and is known to target multiple oncogenes. Some of the genes that are negatively regulated by miR-101 expression include histone methyltransferase EZH2 (enhancer of zeste homolog 2), COX2 (cyclooxygenase-2), POMP (proteasome maturation protein), CERS6, STMN1, MCL-1 and ROCK2, among others. In the present study, we show that miR-101 targets transcriptional coactivator SUB1 homolog (Saccharomyces cerevisiae)/PC4 (positive cofactor 4) and regulates its expression. SUB1 is known to have diverse role in vital cell processes such as DNA replication, repair and heterochromatinization. SUB1 is known to modulate transcription and acts as a mediator between the upstream activators and general transcription machinery. Expression profiling in several cancers revealed SUB1 overexpression, suggesting a potential role in tumorigenesis. However, detailed regulation and function of SUB1 has not been elucidated. In this study, we show elevated expression of SUB1 in aggressive prostate cancer. Knockdown of SUB1 in prostate cancer cells resulted in reduced cell proliferation, invasion and migration in vitro, and tumor growth and metastasis in vivo. Gene expression analyses coupled with chromatin immunoprecipitation revealed that SUB1 binds to the promoter regions of several oncogenes such as PLK1 (Polo-like kinase 1), C-MYC, serine-threonine kinase BUB1B and regulates their expression. Additionally, we observed SUB1 downregulated CDKN1B expression. PLK1 knockdown or use of PLK1 inhibitor can mitigate oncogenic function of SUB1 in benign prostate cancer cells. Thus, our study suggests that miR-101 loss results in increased SUB1 expression and subsequent activation of known oncogenes driving prostate cancer progression and metastasis. This study therefore demonstrates functional role of SUB1 in prostate cancer, and identifies its regulation and potential downstream therapeutic targets of SUB1 in prostate cancer.
Collapse
|
|
28
|
Novel Candidate Biomarkers of Chemoradiosensitivity in Esophageal Squamous Cell Carcinoma: A Systematic Review. Eur Surg Res 2016; 56:141-53. [DOI: 10.1159/000443607] [Citation(s) in RCA: 10] [Impact Index Per Article: 1.3] [Reference Citation Analysis] [Abstract] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 07/16/2015] [Accepted: 12/22/2015] [Indexed: 11/19/2022]
Abstract
There is no doubt that, along with surgery, chemoradiotherapy is an important treatment for esophageal squamous cell carcinoma (ESCC). Patients who respond well to chemoradiotherapy obtain great benefits toward overcoming their cancer, and so a more favorable prognosis. On the other hand, patients who do not respond well have wasted valuable time and experienced severe toxicity and seriously diminished quality of life, only to have their cancer recur with an unfavorable prognosis. For this reason, a reliable biomarker of chemoradiosensitivity in ESCC has long been sought. In this review, we will enumerate recently reported candidate biomarkers of chemoradiosensitivity in ESCC that have the potential for future clinical application.
Collapse
|
|
29
|
Structural analysis and knock-out of a Burkholderia pseudomallei homolog of the eukaryotic transcription coactivator PC4. Gene 2016; 577:140-7. [DOI: 10.1016/j.gene.2015.11.037] [Citation(s) in RCA: 5] [Impact Index Per Article: 0.6] [Reference Citation Analysis] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 08/22/2015] [Revised: 11/20/2015] [Accepted: 11/21/2015] [Indexed: 10/22/2022]
|
|
30
|
XRCC3 is a promising target to improve the radiotherapy effect of esophageal squamous cell carcinoma. Cancer Sci 2015; 106:1678-86. [PMID: 26383967 PMCID: PMC4714664 DOI: 10.1111/cas.12820] [Citation(s) in RCA: 18] [Impact Index Per Article: 2.0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 04/20/2015] [Revised: 08/28/2015] [Accepted: 09/09/2015] [Indexed: 12/18/2022] Open
Abstract
Radiotherapy is widely applied for treatment of esophageal squamous cell carcinoma (ESCC). The Rad51-related protein XRCC3 plays roles in the recombinational repair of DNA double-strand breaks to maintain chromosome stability and repair DNA damage. The present study aimed to investigate the effect of XRCC3 on the radiotherapy response of ESCC and the underlying mechanisms of the roles of XRCC3 in ESCC radiosensitivity. XRCC3 expression in ESCC cells and tissues was higher than that in normal esophageal epithelial cells and corresponding adjacent noncancerous esophageal tissue. High XRCC3 expression was positively correlated with resistance to chemoradiotherapy in ESCC and an independent predictor for short disease-specific survival of ESCC patients. Furthermore, the therapeutic efficacy of radiotherapy in vitro and in vivo was substantially increased by knockdown of XRCC3 in ESCC cells. Ectopic overexpression of XRCC3 in both XRCC3-silenced ESCC cells dramatically enhanced ESCC cells' resistance to radiotherapy. Moreover, radiation resistance conferred by XRCC3 was attributed to enhancement of homologous recombination, maintenance of telomere stability, and a reduction of ESCC cell death by radiation-induced apoptosis and mitotic catastrophe. Our data suggest that XRCC3 protects ESCC cells from ionizing radiation-induced death by promoting DNA damage repair and/or enhancing telomere stability. XRCC3 may be a novel radiosensitivity predictor and promising therapeutic target for ESCC.
Collapse
|
|
31
|
Cooperation between SMYD3 and PC4 drives a distinct transcriptional program in cancer cells. Nucleic Acids Res 2015; 43:8868-83. [PMID: 26350217 PMCID: PMC4605318 DOI: 10.1093/nar/gkv874] [Citation(s) in RCA: 52] [Impact Index Per Article: 5.8] [Reference Citation Analysis] [Abstract] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 04/09/2015] [Accepted: 08/19/2015] [Indexed: 01/17/2023] Open
Abstract
SET and MYND domain containing protein 3 (SMYD3) is a histone methyltransferase, which has been implicated in cell growth and cancer pathogenesis. Increasing evidence suggests that SMYD3 can influence distinct oncogenic processes by acting as a gene-specific transcriptional regulator. However, the mechanistic aspects of SMYD3 transactivation and whether SMYD3 acts in concert with other transcription modulators remain unclear. Here, we show that SMYD3 interacts with the human positive coactivator 4 (PC4) and that such interaction potentiates a group of genes whose expression is linked to cell proliferation and invasion. SMYD3 cooperates functionally with PC4, because PC4 depletion results in the loss of SMYD3-mediated H3K4me3 and target gene expression. Individual depletion of SMYD3 and PC4 diminishes the recruitment of both SMYD3 and PC4, indicating that SMYD3 and PC4 localize at target genes in a mutually dependent manner. Artificial tethering of a SMYD3 mutant incapable of binding to its cognate elements and interacting with PC4 to target genes is sufficient for achieving an active transcriptional state in SMYD3-deficient cells. These observations suggest that PC4 contributes to SMYD3-mediated transactivation primarily by stabilizing SMYD3 occupancy at target genes. Together, these studies define expanded roles for SMYD3 and PC4 in gene regulation and provide an unprecedented documentation of their cooperative functions in stimulating oncogenic transcription.
Collapse
|
|
32
|
Targeting WISP1 to sensitize esophageal squamous cell carcinoma to irradiation. Oncotarget 2015; 6:6218-34. [PMID: 25749038 PMCID: PMC4467433 DOI: 10.18632/oncotarget.3358] [Citation(s) in RCA: 43] [Impact Index Per Article: 4.8] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 10/21/2014] [Accepted: 01/13/2015] [Indexed: 01/12/2023] Open
Abstract
Radiotherapy is a primary treatment modality for esophageal squamous cell carcinoma (ESCC). However, most of patients benefited little from radiotherapy due to refractory radioresistance. We found that WISP1, a downstream target gene of Wnt/β-catenin pathway, was re-expressed in 67.3% of ESCC patients as an oncofetal gene. Expression of WISP1 predicted prognosis of ESCC patients treated with radiotherapy. Overall survival in WISP1-positive patients was significantly poorer than in WISP1-negative patients. Serum concentration of WISP1 after radiotherapy reversely correlated with relapse-free survival. Gain and loss of function studies confirmed that WISP1 mediated radioresistance both in esophageal squamous cancer cells and in xenograft tumor models. Further studies revealed that WISP1 contributed to radioresistance primarily by repressing irradiation-induced DNA damage and activating PI3K kinase. LncRNA BOKAS was up-regulated following radiation and promoted WISP1 expression and resultant radioresistance. Furthermore, WISP1 facilitated its own expression in response to radiation, creating a positive feedback loop and increased radioresistance. Our study revealed WISP1 as a potential target to overcome radioresistance in ESCC.
Collapse
|