|
1
|
Gu X, Chen Y, Cao K, Tu M, Liu W, Ju J. Therapeutic landscape in systemic lupus erythematosus: mtDNA activation of the cGAS-STING pathway. Int Immunopharmacol 2024; 133:112114. [PMID: 38652968 DOI: 10.1016/j.intimp.2024.112114] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/02/2024] [Revised: 04/16/2024] [Accepted: 04/16/2024] [Indexed: 04/25/2024]
Abstract
Mitochondrial DNA (mtDNA) serves as a pivotal immune stimulus in the immune response. During stress, mitochondria release mtDNA into the cytoplasm, where it is recognized by the cytoplasmic DNA receptor cGAS. This activation initiates the cGAS-STING-IRF3 pathway, culminating in an inflammatory response. The cGAS-STING pathway has emerged as a critical mediator of inflammatory responses in microbial infections, stress, autoimmune diseases, chronic illnesses, and tissue injuries. Systemic lupus erythematosus (SLE) is a chronic autoimmune disease characterized by connective tissue involvement across various bodily systems. Its hallmark is the production of numerous autoantibodies, which prompt the immune system to target and damage the body's own tissues, resulting in organ and tissue damage. Increasing evidence implicates the cGAS-STING pathway as a significant contributor to SLE pathogenesis. This article aims to explore the role of the mtDNA-triggered cGAS-STING pathway and its mechanisms in SLE, with the goal of providing novel insights for clinical interventions.
Collapse
Affiliation(s)
- Xiaotian Gu
- School of Basic Medical Sciences, Shandong Second Medical University, Weifang 261053, China
| | - Yong Chen
- School of Basic Medical Sciences, Shandong Second Medical University, Weifang 261053, China
| | - Kunyu Cao
- School of Basic Medical Sciences, Shandong Second Medical University, Weifang 261053, China
| | - Miao Tu
- School of Basic Medical Sciences, Shandong Second Medical University, Weifang 261053, China
| | - Wan Liu
- School of Basic Medical Sciences, Shandong Second Medical University, Weifang 261053, China.
| | - Jiyu Ju
- School of Basic Medical Sciences, Shandong Second Medical University, Weifang 261053, China.
| |
Collapse
|
|
2
|
Hou Y, Yang K, Wang L, Wang J, Huang X, Piffko A, Luo SZ, Yu X, Rao E, Martinez C, Bugno J, Mack M, Vokes EE, Pitroda SP, Chmura SJ, Weichselbaum RR, Liang HL. Radiotherapy Enhances Metastasis Through Immune Suppression by Inducing PD-L1 and MDSC in Distal Sites. Clin Cancer Res 2024; 30:1945-1958. [PMID: 38427437 PMCID: PMC11062826 DOI: 10.1158/1078-0432.ccr-23-3206] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 10/19/2023] [Revised: 01/22/2024] [Accepted: 02/27/2024] [Indexed: 03/03/2024]
Abstract
PURPOSE Radiotherapy (RT) is a widely employed anticancer treatment. Emerging evidence suggests that RT can elicit both tumor-inhibiting and tumor-promoting immune effects. The purpose of this study is to investigate immune suppressive factors of radiotherapy. EXPERIMENTAL DESIGN We used a heterologous two-tumor model in which adaptive concomitant immunity was eliminated. RESULTS Through analysis of PD-L1 expression and myeloid-derived suppressor cells (MDSC) frequencies using patient peripheral blood mononuclear cells and murine two-tumor and metastasis models, we report that local irradiation can induce a systemic increase in MDSC, as well as PD-L1 expression on dendritic cells and myeloid cells, and thereby increase the potential for metastatic dissemination in distal, nonirradiated tissue. In a mouse model using two distinct tumors, we found that PD-L1 induction by ionizing radiation was dependent on elevated chemokine CXCL10 signaling. Inhibiting PD-L1 or MDSC can potentially abrogate RT-induced metastasis and improve clinical outcomes for patients receiving RT. CONCLUSIONS Blockade of PD-L1/CXCL10 axis or MDSC infiltration during irradiation can enhance abscopal tumor control and reduce metastasis.
Collapse
Affiliation(s)
- Yuzhu Hou
- Department of Pathogenic Microbiology and Immunology, School of Basic Medical Sciences, Xi’an Jiaotong University; Xi’an, ShaanXi 710061, China
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
| | - Kaiting Yang
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
| | - Liangliang Wang
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
| | - Jiaai Wang
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
| | - Xiaona Huang
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
| | - Andras Piffko
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
| | - Sean Z. Luo
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
- Current address: Biomedical Engineering program, Northwestern University; Evanston, IL 60201, USA
| | - Xinshuang Yu
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
- Current address: Department of Oncology, First Affiliated Hospital of Shandong, First Medical University and Shandong Provincial Qianfoshan Hospital; Jinan, Shandong 250014, China
| | - Enyu Rao
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
- Current address: Cancer Institute, Xuzhou Medical University; Xuzhou, Jiangsu 221004, China
| | - Carlos Martinez
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
- Current address: University of Illinois at Chicago, Chicago, IL, 60607 USA
| | - Jason Bugno
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
- The Committee on Clinical Pharmacology and Pharmacogenomics, University of Chicago, Chicago, IL 600637, USA
| | - Matthias Mack
- Department of Nephrology, University Hospital Regensburg, 93042 Regensburg, Germany
| | - Everett E. Vokes
- Department of Medicine, University of Chicago, Chicago, IL, 60637 USA
| | - Sean P. Pitroda
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
| | - Steven J. Chmura
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
| | - Ralph R. Weichselbaum
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
| | - Hua Laura Liang
- Department of Radiation and Cellular Oncology, University of Chicago; Chicago, IL 60637 USA
- Ludwig Center for Metastasis Research, University of Chicago; Chicago, IL 60637 USA
| |
Collapse
|
|
3
|
Colangelo NW, Gerber NK, Vatner RE, Cooper BT. Harnessing the cGAS-STING pathway to potentiate radiation therapy: current approaches and future directions. Front Pharmacol 2024; 15:1383000. [PMID: 38659582 PMCID: PMC11039815 DOI: 10.3389/fphar.2024.1383000] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [Track Full Text] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 02/06/2024] [Accepted: 03/15/2024] [Indexed: 04/26/2024] Open
Abstract
In this review, we cover the current understanding of how radiation therapy, which uses ionizing radiation to kill cancer cells, mediates an anti-tumor immune response through the cGAS-STING pathway, and how STING agonists might potentiate this. We examine how cGAS-STING signaling mediates the release of inflammatory cytokines in response to nuclear and mitochondrial DNA entering the cytoplasm. The significance of this in the context of cancer is explored, such as in response to cell-damaging therapies and genomic instability. The contribution of the immune and non-immune cells in the tumor microenvironment is considered. This review also discusses the burgeoning understanding of STING signaling that is independent of inflammatory cytokine release and the various mechanisms by which cancer cells can evade STING signaling. We review the available data on how ionizing radiation stimulates cGAS-STING signaling as well as how STING agonists may potentiate the anti-tumor immune response induced by ionizing radiation. There is also discussion of how novel radiation modalities may affect cGAS-STING signaling. We conclude with a discussion of ongoing and planned clinical trials combining radiation therapy with STING agonists, and provide insights to consider when planning future clinical trials combining these treatments.
Collapse
Affiliation(s)
- Nicholas W. Colangelo
- Department of Radiation Oncology, NYU Grossman School of Medicine, New York, NY, United States
| | - Naamit K. Gerber
- Department of Radiation Oncology, NYU Grossman School of Medicine, New York, NY, United States
| | - Ralph E. Vatner
- Department of Radiation Oncology, University of Cincinnati College of Medicine, Cincinnati, OH, United States
| | - Benjamin T. Cooper
- Department of Radiation Oncology, NYU Grossman School of Medicine, New York, NY, United States
| |
Collapse
|
|
4
|
Hu A, Sun L, Lin H, Liao Y, Yang H, Mao Y. Harnessing innate immune pathways for therapeutic advancement in cancer. Signal Transduct Target Ther 2024; 9:68. [PMID: 38523155 PMCID: PMC10961329 DOI: 10.1038/s41392-024-01765-9] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 09/14/2023] [Revised: 01/18/2024] [Accepted: 02/03/2024] [Indexed: 03/26/2024] Open
Abstract
The innate immune pathway is receiving increasing attention in cancer therapy. This pathway is ubiquitous across various cell types, not only in innate immune cells but also in adaptive immune cells, tumor cells, and stromal cells. Agonists targeting the innate immune pathway have shown profound changes in the tumor microenvironment (TME) and improved tumor prognosis in preclinical studies. However, to date, the clinical success of drugs targeting the innate immune pathway remains limited. Interestingly, recent studies have shown that activation of the innate immune pathway can paradoxically promote tumor progression. The uncertainty surrounding the therapeutic effectiveness of targeted drugs for the innate immune pathway is a critical issue that needs immediate investigation. In this review, we observe that the role of the innate immune pathway demonstrates heterogeneity, linked to the tumor development stage, pathway status, and specific cell types. We propose that within the TME, the innate immune pathway exhibits multidimensional diversity. This diversity is fundamentally rooted in cellular heterogeneity and is manifested as a variety of signaling networks. The pro-tumor effect of innate immune pathway activation essentially reflects the suppression of classical pathways and the activation of potential pro-tumor alternative pathways. Refining our understanding of the tumor's innate immune pathway network and employing appropriate targeting strategies can enhance our ability to harness the anti-tumor potential of the innate immune pathway and ultimately bridge the gap from preclinical to clinical application.
Collapse
Affiliation(s)
- Ankang Hu
- Department of Neurosurgery, Huashan Hospital, Fudan University, Shanghai, P.R. China
- Institute for Translational Brain Research, Shanghai Medical College, Fudan University, Shanghai, P.R. China
- National Center for Neurological Disorders, Huashan Hospital, Shanghai Medical College, Fudan University, Shanghai, P.R. China
- Shanghai Key Laboratory of Brain Function Restoration and Neural Regeneration, Shanghai Clinical Medical Center of Neurosurgery, Neurosurgical Institute of Fudan University, Huashan Hospital, Shanghai Medical College, Fudan University, Shanghai, P.R. China
- State Key Laboratory of Medical Neurobiology and MOE Frontiers Center for Brain Science and MOE Frontiers Center for Brain Science, Institutes of Brain Science, Shanghai Medical College, Fudan University, Shanghai, P.R. China
| | - Li Sun
- Department of Neurosurgery, Huashan Hospital, Fudan University, Shanghai, P.R. China
- National Center for Neurological Disorders, Huashan Hospital, Shanghai Medical College, Fudan University, Shanghai, P.R. China
- Shanghai Key Laboratory of Brain Function Restoration and Neural Regeneration, Shanghai Clinical Medical Center of Neurosurgery, Neurosurgical Institute of Fudan University, Huashan Hospital, Shanghai Medical College, Fudan University, Shanghai, P.R. China
- State Key Laboratory of Medical Neurobiology and MOE Frontiers Center for Brain Science and MOE Frontiers Center for Brain Science, Institutes of Brain Science, Shanghai Medical College, Fudan University, Shanghai, P.R. China
| | - Hao Lin
- Department of Neurosurgery, Huashan Hospital, Fudan University, Shanghai, P.R. China
- National Center for Neurological Disorders, Huashan Hospital, Shanghai Medical College, Fudan University, Shanghai, P.R. China
- Shanghai Key Laboratory of Brain Function Restoration and Neural Regeneration, Shanghai Clinical Medical Center of Neurosurgery, Neurosurgical Institute of Fudan University, Huashan Hospital, Shanghai Medical College, Fudan University, Shanghai, P.R. China
- State Key Laboratory of Medical Neurobiology and MOE Frontiers Center for Brain Science and MOE Frontiers Center for Brain Science, Institutes of Brain Science, Shanghai Medical College, Fudan University, Shanghai, P.R. China
| | - Yuheng Liao
- Shanghai Key Laboratory of Medical Epigenetics, International Co-laboratory of Medical Epigenetics and Metabolism (Ministry of Science and Technology), and Key Laboratory of Metabolism and Molecular Medicine (Ministry of Education), and Molecular and Cell Biology Lab, Institutes of Biomedical Sciences, Shanghai Medical College of Fudan University, Shanghai, P.R. China
| | - Hui Yang
- Department of Neurosurgery, Huashan Hospital, Fudan University, Shanghai, P.R. China.
- Institute for Translational Brain Research, Shanghai Medical College, Fudan University, Shanghai, P.R. China.
- National Center for Neurological Disorders, Huashan Hospital, Shanghai Medical College, Fudan University, Shanghai, P.R. China.
- Shanghai Key Laboratory of Brain Function Restoration and Neural Regeneration, Shanghai Clinical Medical Center of Neurosurgery, Neurosurgical Institute of Fudan University, Huashan Hospital, Shanghai Medical College, Fudan University, Shanghai, P.R. China.
- State Key Laboratory of Medical Neurobiology and MOE Frontiers Center for Brain Science and MOE Frontiers Center for Brain Science, Institutes of Brain Science, Shanghai Medical College, Fudan University, Shanghai, P.R. China.
| | - Ying Mao
- Department of Neurosurgery, Huashan Hospital, Fudan University, Shanghai, P.R. China.
- National Center for Neurological Disorders, Huashan Hospital, Shanghai Medical College, Fudan University, Shanghai, P.R. China.
- Shanghai Key Laboratory of Brain Function Restoration and Neural Regeneration, Shanghai Clinical Medical Center of Neurosurgery, Neurosurgical Institute of Fudan University, Huashan Hospital, Shanghai Medical College, Fudan University, Shanghai, P.R. China.
- State Key Laboratory of Medical Neurobiology and MOE Frontiers Center for Brain Science and MOE Frontiers Center for Brain Science, Institutes of Brain Science, Shanghai Medical College, Fudan University, Shanghai, P.R. China.
| |
Collapse
|
|
5
|
Kawasaki K, Kai K, Minesaki A, Maeda S, Yamauchi M, Kuratomi Y. Chemoradiotherapy and Lymph Node Metastasis Affect Dendritic Cell Infiltration and Maturation in Regional Lymph Nodes of Laryngeal Cancer. Int J Mol Sci 2024; 25:2093. [PMID: 38396770 PMCID: PMC10888629 DOI: 10.3390/ijms25042093] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/17/2024] [Revised: 02/05/2024] [Accepted: 02/07/2024] [Indexed: 02/25/2024] Open
Abstract
Dendritic cells (DCs) are the most specialized antigen-presenting cells, and lymph nodes (LNs) play an important role in the DC-mediated T-cell response. We evaluated the infiltration of CD1a-positive DCs (CD1a-DCs), i.e., immature DCs, and S100-positive dendritic cells (S100-DCs), a mixture of immature and mature DCs, in 73 cases of laryngeal cancer and its regional LNs. Among them, 31 patients underwent radiotherapy (RT) or chemoradiotherapy (CRT) prior to surgery. No significant difference was found for CD1a-DC infiltration in the primary tumors, metastatic LNs and non-metastatic LNs, while S100-DCs were significantly fewer in number in the primary tumors and metastatic LNs compared to non-metastatic LNs. The cases which showed a high infiltration of S100-DCs in the metastatic LNs appeared to show a favorable prognosis, although statistical significance was not reached. In the RT/CRT group, the infiltration of the CD1a-DCs and S100-DCs was less in the primary tumors and metastatic LNs compared to the treatment-naive group. Conversely, the RT/CRT group showed higher CD1a-DC and S100-DC numbers in the non-metastatic LNs compared to the treatment-naïve group. Thus, DC maturation in metastatic LNs plays an important role in tumor immunity in laryngeal cancer, and the infiltration of DCs into the primary tumor and metastatic LNs is impaired by RT/CRT.
Collapse
Affiliation(s)
- Kanako Kawasaki
- Department of Pathology & Microbiology, Faculty of Medicine, Saga University, Saga 849-8501, Japan; (K.K.); (S.M.)
- Department of Otolaryngology—Head & Neck Surgery, Faculty of Medicine, Saga University, Saga 849-8501, Japan; (A.M.); (M.Y.); (Y.K.)
| | - Keita Kai
- Department of Pathology, Saga University Hospital, Saga 849-8501, Japan
| | - Akimichi Minesaki
- Department of Otolaryngology—Head & Neck Surgery, Faculty of Medicine, Saga University, Saga 849-8501, Japan; (A.M.); (M.Y.); (Y.K.)
| | - Sachiko Maeda
- Department of Pathology & Microbiology, Faculty of Medicine, Saga University, Saga 849-8501, Japan; (K.K.); (S.M.)
| | - Moriyasu Yamauchi
- Department of Otolaryngology—Head & Neck Surgery, Faculty of Medicine, Saga University, Saga 849-8501, Japan; (A.M.); (M.Y.); (Y.K.)
| | - Yuichiro Kuratomi
- Department of Otolaryngology—Head & Neck Surgery, Faculty of Medicine, Saga University, Saga 849-8501, Japan; (A.M.); (M.Y.); (Y.K.)
| |
Collapse
|
|
6
|
Ma L, Deng L, Peng J, Yu J, Meng X. Chemotherapy-free radiotherapy combined with immune checkpoint inhibitors: a new regimen for locally advanced non-small cell lung cancer? Cancer Biol Med 2024; 20:j.issn.2095-3941.2023.0402. [PMID: 38318930 PMCID: PMC10845940 DOI: 10.20892/j.issn.2095-3941.2023.0402] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 11/01/2023] [Accepted: 12/22/2023] [Indexed: 02/07/2024] Open
Abstract
Maintenance immunotherapy after concurrent chemoradiotherapy remains the standard therapeutic approach in patients with unresectable locally advanced non-small cell lung cancer (LA-NSCLC). The efficacy of pembrolizumab without chemotherapy in stage IV NSCLC has incited interest in similar approaches for LA-NSCLC. Several recent investigations involving the synergistic potential of immunotherapy combined with radiotherapy (iRT) have generated encouraging results. This review discusses the existing studies and prospective directions of chemotherapy-free iRT strategies in unresectable LA-NSCLC. Although the initial findings of chemotherapy-free iRT strategies have shown promising efficacy, we must consider the methodologic limitations of current studies and the myriad of challenges that accompany the implementation of chemotherapy-free iRT. These challenges include determining the optimal dose and fractionation, precise target volume delineation, and identification of additional suitable patient cohorts. Furthermore, the feasibility of chemotherapy-free iRT as a novel treatment modality for select patients with LA-NSCLC is contingent upon validation through randomized phase III trials.
Collapse
Affiliation(s)
- Lin Ma
- Department of Oncology, Renmin Hospital of Wuhan University, Wuhan 430000, China
- Department of Radiation Oncology, Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, Jinan 250117, China
| | - Liufu Deng
- School of Pharmacy, Shanghai Jiao Tong University, Shanghai 200240, China
| | - Jianfeng Peng
- Department of Radiation Oncology, Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, Jinan 250117, China
| | - Jinming Yu
- Department of Oncology, Renmin Hospital of Wuhan University, Wuhan 430000, China
- Department of Radiation Oncology, Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, Jinan 250117, China
| | - Xiangjiao Meng
- Department of Radiation Oncology, Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, Jinan 250117, China
| |
Collapse
|
|
7
|
Hu Y, Ye R, Su J, Rui Y, Yu XF. cGAS-STING-mediated novel nonclassic antiviral activities. J Med Virol 2024; 96:e29403. [PMID: 38293806 DOI: 10.1002/jmv.29403] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 10/28/2023] [Revised: 12/13/2023] [Accepted: 01/04/2024] [Indexed: 02/01/2024]
Abstract
Stimulatorof interferon genes (STING) is an intracellular sensor of cyclic dinucleotides involved in the innate immune response against pathogen- or self-derived DNA. For years, interferon (IFN) induction of cyclic GMP-AMP synthase (cGAS)-STING has been considered as a canonical pattern defending the host from viral invasion. The mechanism of the cGAS-STING-IFN pathway has been well-illustrated. However, other signalling cascades driven by cGAS-STING have emerged in recent years and some of them have been found to possess antiviral ability independent of IFN. Here, we summarize the current progress on cGAS-STING-mediated nonclassic antiviral activities with an emphasis on the nuclear factor-κB and autophagy pathways, which are the most-studied pathways. In addition, we briefly present the primordial function of the cGAS-STING pathway in primitive species to show the importance of IFN-unrelated antiviral activity from an evolutionary angle. Finally, we discuss open questions that need to be solved for further exploitation of this field.
Collapse
Affiliation(s)
- Ying Hu
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, China National Ministry of Education, Key Laboratory of Molecular Biology in Medical Sciences, Zhejiang Province, China), The Second Affiliated Hospital, Zhejiang University School of Medicine; Zhejiang Provincial Clinical Research Center for Cancer, Hangzhou, Zhejiang, China
| | - Runxin Ye
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, China National Ministry of Education, Key Laboratory of Molecular Biology in Medical Sciences, Zhejiang Province, China), The Second Affiliated Hospital, Zhejiang University School of Medicine; Zhejiang Provincial Clinical Research Center for Cancer, Hangzhou, Zhejiang, China
| | - Jiaming Su
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, China National Ministry of Education, Key Laboratory of Molecular Biology in Medical Sciences, Zhejiang Province, China), The Second Affiliated Hospital, Zhejiang University School of Medicine; Zhejiang Provincial Clinical Research Center for Cancer, Hangzhou, Zhejiang, China
- Cancer Center, Zhejiang University, Hangzhou, Zhejiang, China
| | - Yajuan Rui
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, China National Ministry of Education, Key Laboratory of Molecular Biology in Medical Sciences, Zhejiang Province, China), The Second Affiliated Hospital, Zhejiang University School of Medicine; Zhejiang Provincial Clinical Research Center for Cancer, Hangzhou, Zhejiang, China
- Cancer Center, Zhejiang University, Hangzhou, Zhejiang, China
| | - Xiao-Fang Yu
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, China National Ministry of Education, Key Laboratory of Molecular Biology in Medical Sciences, Zhejiang Province, China), The Second Affiliated Hospital, Zhejiang University School of Medicine; Zhejiang Provincial Clinical Research Center for Cancer, Hangzhou, Zhejiang, China
- Cancer Center, Zhejiang University, Hangzhou, Zhejiang, China
| |
Collapse
|
|
8
|
Peng C, Ye Z, Ju Y, Huang X, Zhan C, Wei K, Zhang Z. Mechanism of action and treatment of type I interferon in hepatocellular carcinoma. Clin Transl Oncol 2024; 26:326-337. [PMID: 37402970 DOI: 10.1007/s12094-023-03266-7] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 03/16/2023] [Accepted: 06/25/2023] [Indexed: 07/06/2023]
Abstract
Hepatocellular carcinoma (HCC) caused by HBV, HCV infection, and other factors is one of the most common malignancies in the world. Although, percutaneous treatments such as surgery, ethanol injection, radiofrequency ablation, and transcatheter treatments such as arterial chemoembolization are useful for local tumor control, they are not sufficient to improve the prognosis of patients with HCC. External interferon agents that induce interferon-related genes or type I interferon in combination with other drugs can reduce the recurrence rate and improve survival in HCC patients after surgery. Therefore, in this review, we focus on recent advances in the mechanism of action of type I interferons, emerging therapies, and potential therapeutic strategies for the treatment of HCC using IFNs.
Collapse
Affiliation(s)
- Chunxiu Peng
- State Key Laboratory of Targeting Oncology, National Center for International Research of Bio-targeting Theranostics, Guangxi Key Laboratory of Bio-targeting Theranostics, Collaborative Innovation Center for Targeting Tumor Diagnosis and Therapy, Guangxi Medical University, Nanning, 530021, Guangxi, China
| | - Zhijian Ye
- State Key Laboratory of Targeting Oncology, National Center for International Research of Bio-targeting Theranostics, Guangxi Key Laboratory of Bio-targeting Theranostics, Collaborative Innovation Center for Targeting Tumor Diagnosis and Therapy, Guangxi Medical University, Nanning, 530021, Guangxi, China
| | - Ying Ju
- State Key Laboratory of Targeting Oncology, National Center for International Research of Bio-targeting Theranostics, Guangxi Key Laboratory of Bio-targeting Theranostics, Collaborative Innovation Center for Targeting Tumor Diagnosis and Therapy, Guangxi Medical University, Nanning, 530021, Guangxi, China
| | - Xiuxin Huang
- State Key Laboratory of Targeting Oncology, National Center for International Research of Bio-targeting Theranostics, Guangxi Key Laboratory of Bio-targeting Theranostics, Collaborative Innovation Center for Targeting Tumor Diagnosis and Therapy, Guangxi Medical University, Nanning, 530021, Guangxi, China
| | - Chenjie Zhan
- State Key Laboratory of Targeting Oncology, National Center for International Research of Bio-targeting Theranostics, Guangxi Key Laboratory of Bio-targeting Theranostics, Collaborative Innovation Center for Targeting Tumor Diagnosis and Therapy, Guangxi Medical University, Nanning, 530021, Guangxi, China
| | - Ke Wei
- State Key Laboratory of Targeting Oncology, National Center for International Research of Bio-targeting Theranostics, Guangxi Key Laboratory of Bio-targeting Theranostics, Collaborative Innovation Center for Targeting Tumor Diagnosis and Therapy, Guangxi Medical University, Nanning, 530021, Guangxi, China
| | - Zhiyong Zhang
- State Key Laboratory of Targeting Oncology, National Center for International Research of Bio-targeting Theranostics, Guangxi Key Laboratory of Bio-targeting Theranostics, Collaborative Innovation Center for Targeting Tumor Diagnosis and Therapy, Guangxi Medical University, Nanning, 530021, Guangxi, China.
| |
Collapse
|
|
9
|
Shen Q, Xu P, Mei C. Role of micronucleus-activated cGAS-STING signaling in antitumor immunity. Zhejiang Da Xue Xue Bao Yi Xue Ban 2024; 53:25-34. [PMID: 38273467 PMCID: PMC10945493 DOI: 10.3724/zdxbyxb-2023-0485] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 10/08/2023] [Accepted: 12/12/2023] [Indexed: 01/27/2024]
Abstract
Cyclic guanosine monophosphate-adenosine monophosphate synthase (cGAS)-stimulator of interferon genes (STING) signaling is a significant component of the innate immune system and functions as a vital sentinel mechanism to monitor cellular and tissue aberrations in microbial invasion and organ injury. cGAS, a cytosolic DNA sensor, is specialized in recognizing abnormally localized cytoplasmic double-stranded DNA (dsDNA) and catalyzes the formation of a second messenger cyclic-GMP-AMP (cGAMP), which initiates a cascade of type Ⅰ interferon and inflammatory responses mediated by STING. Micronucleus, a byproduct of chromosomal missegregation during anaphase, is also a significant contributor to cytoplasmic dsDNA. These unstable subcellular structures are susceptible to irreversible nuclear envelope rupture, exposing genomic dsDNA to the cytoplasm, which potently recruits cGAS and activates STING-mediated innate immune signaling and its downstream activities, including type Ⅰ interferon and classical nuclear factor-κB (NF-κB) signaling pathways lead to senescence, apoptosis, autophagy activating anti-cancer immunity or directly killing tumor cells. However, sustained STING activation-induced endoplasmic reticulum stress, activated chronic type Ⅰ interferon and nonclassical NF-κB signaling pathways remodel immunosuppressive tumor microenvironment, leading to immune evasion and facilitating tumor metastasis. Therefore, activated cGAS-STING signaling plays a dual role of suppressing or facilitating tumor growth in tumorigenesis and therapy. This review elaborates on research advances in mechanisms of micronucleus inducing activation of cGAS-STING signaling and its implications in tumorigenesis and therapeutic strategies of malignant tumors.
Collapse
Affiliation(s)
- Qin Shen
- Life Sciences Institute, Zhejiang University, Hangzhou 310058, China.
| | - Pinglong Xu
- Life Sciences Institute, Zhejiang University, Hangzhou 310058, China.
- Key Laboratory of Biosystems Homeostasis and Protection, Ministry of Education, Zhejiang Provincial Key Laboratory for Cancer Molecular Cell Biology, Zhejiang University, Hangzhou 310058, China.
- Institute of Intelligent Medicine, Hangzhou Global Scientific and Technological Innovation Center, Zhejiang University, Hangzhou 311200, China.
- Cancer Center, Zhejiang University, Hangzhou 310058, China.
| | - Chen Mei
- Life Sciences Institute, Zhejiang University, Hangzhou 310058, China.
- Institute of Intelligent Medicine, Hangzhou Global Scientific and Technological Innovation Center, Zhejiang University, Hangzhou 311200, China.
| |
Collapse
|
|
10
|
Zhang J, Yu S, Peng Q, Wang P, Fang L. Emerging mechanisms and implications of cGAS-STING signaling in cancer immunotherapy strategies. Cancer Biol Med 2024; 21:j.issn.2095-3941.2023.0440. [PMID: 38172538 PMCID: PMC10875285 DOI: 10.20892/j.issn.2095-3941.2023.0440] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 11/13/2023] [Accepted: 12/14/2023] [Indexed: 01/05/2024] Open
Abstract
The intricate interplay between the human immune system and cancer development underscores the central role of immunotherapy in cancer treatment. Within this landscape, the innate immune system, a critical sentinel protecting against tumor incursion, is a key player. The cyclic GMP-AMP synthase (cGAS) and stimulator of interferon genes (STING) pathway has been found to be a linchpin of innate immunity: activation of this signaling pathway orchestrates the production of type I interferon (IFN-α/β), thus fostering the maturation, differentiation, and mobilization of immune effectors in the tumor microenvironment. Furthermore, STING activation facilitates the release and presentation of tumor antigens, and therefore is an attractive target for cancer immunotherapy. Current strategies to activate the STING pathway, including use of pharmacological agonists, have made substantial advancements, particularly when combined with immune checkpoint inhibitors. These approaches have shown promise in preclinical and clinical settings, by enhancing patient survival rates. This review describes the evolving understanding of the cGAS-STING pathway's involvement in tumor biology and therapy. Moreover, this review explores classical and non-classical STING agonists, providing insights into their mechanisms of action and potential for optimizing immunotherapy strategies. Despite challenges and complexities, the cGAS-STING pathway, a promising avenue for enhancing cancer treatment efficacy, has the potential to revolutionize patient outcomes.
Collapse
Affiliation(s)
- Jiawen Zhang
- Tongji University Cancer Center, Shanghai Tenth People’s Hospital, School of Medicine, Tongji University, Shanghai 200072, China
- Reproductive Medicine Center, Department of Obstetrics and Gynecology, Shanghai General Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai 201620, China
| | - Sihui Yu
- Department of Obstetrics and Gynecology, Zhongshan Hospital, Fudan University, Shanghai 200032, China
| | - Qiao Peng
- Tongji University Cancer Center, Shanghai Tenth People’s Hospital, School of Medicine, Tongji University, Shanghai 200072, China
| | - Ping Wang
- Tongji University Cancer Center, Shanghai Tenth People’s Hospital, School of Medicine, Tongji University, Shanghai 200072, China
| | - Lan Fang
- Tongji University Cancer Center, Shanghai Tenth People’s Hospital, School of Medicine, Tongji University, Shanghai 200072, China
| |
Collapse
|
|
11
|
Zhao M, Wang T, Gleber-Netto FO, Chen Z, McGrail DJ, Gomez JA, Ju W, Gadhikar MA, Ma W, Shen L, Wang Q, Tang X, Pathak S, Raso MG, Burks JK, Lin SY, Wang J, Multani AS, Pickering CR, Chen J, Myers JN, Zhou G. Mutant p53 gains oncogenic functions through a chromosomal instability-induced cytosolic DNA response. Nat Commun 2024; 15:180. [PMID: 38167338 PMCID: PMC10761733 DOI: 10.1038/s41467-023-44239-2] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/04/2023] [Accepted: 12/05/2023] [Indexed: 01/05/2024] Open
Abstract
Inactivating TP53 mutations leads to a loss of function of p53, but can also often result in oncogenic gain-of-function (GOF) of mutant p53 (mutp53) proteins which promotes tumor development and progression. The GOF activities of TP53 mutations are well documented, but the mechanisms involved remain poorly understood. Here, we study the mutp53 interactome and find that by targeting minichromosome maintenance complex components (MCMs), GOF mutp53 predisposes cells to replication stress and chromosomal instability (CIN), leading to a tumor cell-autonomous and cyclic GMP-AMP synthase (cGAS)-stimulator of interferon genes (STING)-dependent cytosolic DNA response that activates downstream non-canonical nuclear factor kappa light chain enhancer of activated B cell (NC-NF-κB) signaling. Consequently, GOF mutp53-MCMs-CIN-cytosolic DNA-cGAS-STING-NC-NF-κB signaling promotes tumor cell metastasis and an immunosuppressive tumor microenvironment through antagonizing interferon signaling and regulating genes associated with pro-tumorigenic inflammation. Our findings have important implications for understanding not only the GOF activities of TP53 mutations but also the genome-guardian role of p53 and its inactivation during tumor development and progression.
Collapse
Affiliation(s)
- Mei Zhao
- Department of Head and Neck Surgery, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Tianxiao Wang
- Department of Head and Neck Surgery, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
- Department of Head and Neck Surgery, Key Laboratory of Carcinogenesis and Translational Research, Peking University Cancer Hospital & Institute, 100142, Beijing, China
| | - Frederico O Gleber-Netto
- Department of Head and Neck Surgery, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Zhen Chen
- Department of Experimental Radiation Oncology, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Daniel J McGrail
- Department of Systems Biology, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
- Center for Immunotherapy and Precision Immuno-Oncology, Cleveland Clinic, Cleveland, OH, 44195, USA
- Lerner Research Institute, Cleveland Clinic, Cleveland, OH, 44195, USA
| | - Javier A Gomez
- Department of Leukemia, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Wutong Ju
- Department of Head and Neck Surgery, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Mayur A Gadhikar
- Department of Head and Neck Surgery, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Wencai Ma
- Department of Bioinformatics and Computational Biology, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Li Shen
- Department of Bioinformatics and Computational Biology, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Qi Wang
- Department of Bioinformatics and Computational Biology, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Ximing Tang
- Department of Translational Molecular Pathology, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Sen Pathak
- Department of Genetics, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Maria Gabriela Raso
- Department of Translational Molecular Pathology, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Jared K Burks
- Department of Leukemia, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Shiaw-Yih Lin
- Department of Systems Biology, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Jing Wang
- Department of Bioinformatics and Computational Biology, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Asha S Multani
- Department of Genetics, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Curtis R Pickering
- Department of Head and Neck Surgery, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
- Department of Surgery-Otolaryngology, Yale School of Medicine, New Haven, CT, 06250, USA
| | - Junjie Chen
- Department of Experimental Radiation Oncology, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA
| | - Jeffrey N Myers
- Department of Head and Neck Surgery, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA.
| | - Ge Zhou
- Department of Head and Neck Surgery, The University of Texas MD Anderson Cancer Center, Houston, TX, 77030, USA.
| |
Collapse
|
|
12
|
Kim J, Pena JV, McQueen HP, Kong L, Michael D, Lomashvili EM, Cook PR. Downstream STING pathways IRF3 and NF-κB differentially regulate CCL22 in response to cytosolic dsDNA. Cancer Gene Ther 2024; 31:28-42. [PMID: 37990062 DOI: 10.1038/s41417-023-00678-z] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 11/11/2022] [Revised: 08/22/2023] [Accepted: 10/11/2023] [Indexed: 11/23/2023]
Abstract
Double-stranded DNA (dsDNA) in the cytoplasm of eukaryotic cells is abnormal and typically indicates the presence of pathogens or mislocalized self-DNA. Multiple sensors detect cytosolic dsDNA and trigger robust immune responses via activation of type I interferons. Several cancer immunotherapy treatments also activate cytosolic nucleic acid sensing pathways, including oncolytic viruses, nucleic acid-based cancer vaccines, and pharmacological agonists. We report here that cytosolic dsDNA introduced into malignant cells can robustly upregulate expression of CCL22, a chemokine responsible for the recruitment of regulatory T cells (Tregs). Tregs in the tumor microenvironment are thought to repress anti-tumor immune responses and contribute to tumor immune evasion. Surprisingly, we found that CCL22 upregulation by dsDNA was mediated primarily by interferon regulatory factor 3 (IRF3), a key transcription factor that activates type I interferons. This finding was unexpected given previous reports that type I interferon alpha (IFN-α) inhibits CCL22 and that IRF3 is associated with strong anti-tumor immune responses, not Treg recruitment. We also found that CCL22 upregulation by dsDNA occurred concurrently with type I interferon beta (IFN-β) upregulation. IRF3 is one of two transcription factors downstream of the STimulator of INterferon Genes (STING), a hub adaptor protein through which multiple dsDNA sensors transmit their signals. The other transcription factor downstream of STING, NF-κB, has been reported to regulate CCL22 expression in other contexts, and NF-κB has also been associated with multiple pro-tumor functions, including Treg recruitment. However, we found that NF-κB in the context of activation by cytosolic dsDNA contributed minimally to CCL22 upregulation compared with IRF3. Lastly, we observed that two strains of the same cell line differed profoundly in their capacity to upregulate CCL22 and IFN-β in response to dsDNA, despite apparent STING activation in both cell lines. This finding suggests that during tumor evolution, cells can acquire, or lose, the ability to upregulate CCL22. This study adds to our understanding of factors that may modulate immune activation in response to cytosolic DNA and has implications for immunotherapy strategies that activate DNA sensing pathways in cancer cells.
Collapse
Affiliation(s)
- Jihyun Kim
- Department of Biomedical Sciences, Mercer University School of Medicine, Macon, GA, USA
| | - Jocelyn V Pena
- Department of Biomedical Sciences, Mercer University School of Medicine, Macon, GA, USA
| | - Hannah P McQueen
- Department of Biomedical Sciences, Mercer University School of Medicine, Macon, GA, USA
| | - Lingwei Kong
- Department of Biomedical Sciences, Mercer University School of Medicine, Macon, GA, USA
| | - Dina Michael
- Department of Biomedical Sciences, Mercer University School of Medicine, Macon, GA, USA
| | - Elmira M Lomashvili
- Department of Biomedical Sciences, Mercer University School of Medicine, Macon, GA, USA
| | - Pamela R Cook
- Department of Biomedical Sciences, Mercer University School of Medicine, Macon, GA, USA.
| |
Collapse
|
|
13
|
Wang L, Katipally RR, Liang HL, Yang K, Pitroda SP, He C, Weichselbaum RR. RNA m 6A methylation and MDSCs: Roles and therapeutic implications for radiotherapy. Med 2023; 4:863-874. [PMID: 38070481 PMCID: PMC10751059 DOI: 10.1016/j.medj.2023.09.001] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 07/13/2023] [Revised: 08/29/2023] [Accepted: 09/13/2023] [Indexed: 12/18/2023]
Abstract
Emerging evidence suggests that local tumor radiotherapy reshapes the repertoire of circulating myeloid-derived suppressor cells (MDSCs) and leads to their infiltration into the tumor microenvironment, which poses a major obstacle for radiotherapy efficacy. Recent findings have identified RNA m6A modification at the nexus of both anti-tumor immunity and radiation response. Here, we examine the mechanisms by which this RNA modification modulates the immune milieu of the radiation-remodeled tumor microenvironment. We discuss potential therapeutic interventions targeting m6A machinery to improve radiotherapy response.
Collapse
Affiliation(s)
- Liangliang Wang
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA.
| | - Rohan R Katipally
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA
| | - Hua Laura Liang
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA
| | - Kaiting Yang
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA
| | - Sean P Pitroda
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA
| | - Chuan He
- Department of Chemistry, Department of Biochemistry and Molecular Biology, and Institute for Biophysical Dynamics, The University of Chicago, Chicago, IL 60637, USA; Howard Hughes Medical Institute, University of Chicago, Chicago, IL 60637, USA
| | - Ralph R Weichselbaum
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA.
| |
Collapse
|
|
14
|
Wang J, Wu M, Sun J, Chen M, Zhang Z, Yu J, Chen D. Pan-cancer analysis identifies protein arginine methyltransferases PRMT1 and PRMT5 and their related signatures as markers associated with prognosis, immune profile, and therapeutic response in lung adenocarcinoma. Heliyon 2023; 9:e22088. [PMID: 38125466 PMCID: PMC10731011 DOI: 10.1016/j.heliyon.2023.e22088] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 08/08/2023] [Revised: 11/02/2023] [Accepted: 11/03/2023] [Indexed: 12/23/2023] Open
Abstract
Purpose Protein arginine methyltransferases (PRMTs) regulate several signal transduction pathways involved in cancer progression. Recently, it has been reported that PRMTs are closely related to anti-tumor immunity; however, the underlying mechanisms have yet to be studied in lung adenocarcinoma (LUAD). In this study, we focused on PRMT1 and PRMT5, key members of the PRMT family. And their signatures in lung carcinoma associated with prognosis, immune profile, and therapeutic response including immunotherapy and radiotherapy were explored. Methods To understand the function of PRMT1 and PRMT5 in tumor cells, we examined the association between the expression of PRMT1 and PRMT5 and the clinical, genomic, and immune characteristics, as well as the sensitivity to immunotherapy and radiotherapy. Specifically, our investigation focused on the role of PRMT1 and PRMT5 in tumor progression, with particular emphasis on interferon-stimulated genes (ISGs) and the pathway of type I interferon. Furthermore, the influence of proliferation, migration, and invasion ability was investigated based on the expression of PRMT1 and PRMT5 in human lung adenocarcinoma cell lines. Results Through the examination of receiver operating characteristic (ROC) and survival studies, PRMT1 and PRMT5 were identified as potential biomarkers for the diagnosis and prognosis. Additionally, heightened expression of PRMT1 or PRMT5 was associated with immunosuppressive microenvironments. Furthermore, a positive correlation was observed between the presence of PRMT1 or PRMT5 with microsatellite instability, tumor mutational burden, and neoantigens in the majority of cancers. Moreover, the predictive potential of PRMT1 or PRMT5 in individuals undergoing immunotherapy has been acknowledged. Our study ultimately revealed that the inhibition of PRMT1 and PRMT5 in lung adenocarcinoma resulted in the activation of the cGAS-STING pathway, especially after radiation. Favorable prognosis was observed in lung adenocarcinoma patients receiving radiotherapy with reduced PRMT1 or PRMT5 expression. It was also found that the expression of PRMT1 and PRMT5 influenced proliferation, migration, and invasion of human lung adenocarcinoma cell lines. Conclusion The findings indicate that PRMT1 and PRMT5 exhibit potential as immune-related biomarkers for the diagnosis and prognosis of cancer. Furthermore, these biomarkers could be therapeutically targeted to augment the efficacy of immunotherapy and radiotherapy in lung adenocarcinoma.
Collapse
Affiliation(s)
- Jia Wang
- Shantou University Medical College, Shantou, 515041, Guangdong Province, China
- Department of Radiation Oncology and Shandong Provincial Key Laboratory of Radiation Oncology, Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, 250117, Jinan, Shandong Province, China
| | - Meng Wu
- Department of Radiation Oncology and Shandong Provincial Key Laboratory of Radiation Oncology, Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, 250117, Jinan, Shandong Province, China
| | - Jujie Sun
- Department of Pathology, Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, 250117, Jinan, Shandong Province, China
| | - Minxin Chen
- Department of Radiation Oncology and Shandong Provincial Key Laboratory of Radiation Oncology, Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, 250117, Jinan, Shandong Province, China
- Department of Oncology, The Affiliated Hospital of Southwest Medical University, Luzhou, Sichuan, China
| | - Zengfu Zhang
- Department of Radiation Oncology and Shandong Provincial Key Laboratory of Radiation Oncology, Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, 250117, Jinan, Shandong Province, China
| | - Jinming Yu
- Department of Radiation Oncology and Shandong Provincial Key Laboratory of Radiation Oncology, Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, 250117, Jinan, Shandong Province, China
| | - Dawei Chen
- Department of Radiation Oncology and Shandong Provincial Key Laboratory of Radiation Oncology, Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, 250117, Jinan, Shandong Province, China
| |
Collapse
|
|
15
|
Korneenko TV, Pestov NB, Nevzorov IA, Daks AA, Trachuk KN, Solopova ON, Barlev NA. At the Crossroads of the cGAS-cGAMP-STING Pathway and the DNA Damage Response: Implications for Cancer Progression and Treatment. Pharmaceuticals (Basel) 2023; 16:1675. [PMID: 38139802 PMCID: PMC10747911 DOI: 10.3390/ph16121675] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 09/30/2023] [Revised: 11/21/2023] [Accepted: 11/21/2023] [Indexed: 12/24/2023] Open
Abstract
The evolutionary conserved DNA-sensing cGAS-STING innate immunity pathway represents one of the most important cytosolic DNA-sensing systems that is activated in response to viral invasion and/or damage to the integrity of the nuclear envelope. The key outcome of this pathway is the production of interferon, which subsequently stimulates the transcription of hundreds of genes. In oncology, the situation is complex because this pathway may serve either anti- or pro-oncogenic roles, depending on context. The prevailing understanding is that when the innate immune response is activated by sensing cytosolic DNA, such as DNA released from ruptured micronuclei, it results in the production of interferon, which attracts cytotoxic cells to destroy tumors. However, in tumor cells that have adjusted to significant chromosomal instability, particularly in relapsed, treatment-resistant cancers, the cGAS-STING pathway often supports cancer progression, fostering the epithelial-to-mesenchymal transition (EMT). Here, we review this intricate pathway in terms of its association with cancer progression, giving special attention to pancreatic ductal adenocarcinoma and gliomas. As the development of new cGAS-STING-modulating small molecules and immunotherapies such as oncolytic viruses involves serious challenges, we highlight several recent fundamental discoveries, such as the proton-channeling function of STING. These discoveries may serve as guiding lights for potential pharmacological advancements.
Collapse
Affiliation(s)
- Tatyana V. Korneenko
- Group of Cross-Linking Enzymes, Shemyakin-Ovchinnikov Institute of Bioorganic Chemistry, Moscow 117997, Russia
| | - Nikolay B. Pestov
- Group of Cross-Linking Enzymes, Shemyakin-Ovchinnikov Institute of Bioorganic Chemistry, Moscow 117997, Russia
- Institute of Biomedical Chemistry, Moscow 119121, Russia
- Chumakov Federal Scientific Center for Research and Development of Immune-and-Biological Products, Moscow 108819, Russia
| | - Ivan A. Nevzorov
- Institute of Cytology, Tikhoretsky ave 4, St-Petersburg 194064, Russia
| | - Alexandra A. Daks
- Institute of Cytology, Tikhoretsky ave 4, St-Petersburg 194064, Russia
| | - Kirill N. Trachuk
- Chumakov Federal Scientific Center for Research and Development of Immune-and-Biological Products, Moscow 108819, Russia
| | - Olga N. Solopova
- Research Institute of Experimental Diagnostics and Tumor Therapy, Blokhin National Medical Research Center of Oncology, Moscow 115478, Russia
| | - Nickolai A. Barlev
- Institute of Biomedical Chemistry, Moscow 119121, Russia
- Chumakov Federal Scientific Center for Research and Development of Immune-and-Biological Products, Moscow 108819, Russia
- Institute of Cytology, Tikhoretsky ave 4, St-Petersburg 194064, Russia
- Institute of Translational Medicine and Biotechnology, Sechenov First Moscow State Medical University, Moscow 119991, Russia
| |
Collapse
|
|
16
|
Zhao K, Huang J, Zhao Y, Wang S, Xu J, Yin K. Targeting STING in cancer: Challenges and emerging opportunities. Biochim Biophys Acta Rev Cancer 2023; 1878:188983. [PMID: 37717857 DOI: 10.1016/j.bbcan.2023.188983] [Citation(s) in RCA: 2] [Impact Index Per Article: 2.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 06/22/2023] [Revised: 08/21/2023] [Accepted: 08/26/2023] [Indexed: 09/19/2023]
Abstract
The cyclic GMP-AMP synthase (cGAS)-stimulator of interferon genes (STING) signaling pathway is a key pathway through which the host regulates immune responses by recognizing cytoplasmic double-stranded DNA of abnormal origin, and it plays an important role in tumor growth as well as metastasis, with relevant molecular details constantly being explored and updated. The significant immunomodulatory effects make STING an attractive target for cancer immunotherapy, and STING agonists have been receiving great attention for their development and clinical translation. Despite exciting results in preclinical work, the application of STING agonists to cancer therapy remains challenging due to their poor pharmacokinetic and physicochemical properties, as well as toxic side effects they produce. Here, we summarize the dichotomous role of cGAS-STING in cancer and discuss the limitations of cancer immunotherapy based on STING activation as well as feasible strategies to overcome them to achieve tumor regression.
Collapse
Affiliation(s)
- Kexin Zhao
- Department of General Surgery, Affiliated Hospital of Jiangsu University, Zhenjiang, Jiangsu, China; Department of Immunology, Jiangsu Key Laboratory of Laboratory Medicine, School of Medicine, Jiangsu University, Zhenjiang, China
| | - Jiaojiao Huang
- Department of Immunology, Jiangsu Key Laboratory of Laboratory Medicine, School of Medicine, Jiangsu University, Zhenjiang, China
| | - Yue Zhao
- Department of Immunology, Jiangsu Key Laboratory of Laboratory Medicine, School of Medicine, Jiangsu University, Zhenjiang, China
| | - Shengjun Wang
- Department of Immunology, Jiangsu Key Laboratory of Laboratory Medicine, School of Medicine, Jiangsu University, Zhenjiang, China; Department of Laboratory Medicine, the Affiliated People's Hospital, Jiangsu University, Zhenjiang, China.
| | - Juan Xu
- Department of Laboratory Medicine, The Affiliated Taizhou People's Hospital of Nanjing Medical University, Taizhou, China.
| | - Kai Yin
- Department of General Surgery, Affiliated Hospital of Jiangsu University, Zhenjiang, Jiangsu, China.
| |
Collapse
|
|
17
|
Lan Y, Pi W, Zhou Z, Meng Y, DanMei, Xu Y, Xia X, WeiWang, Yang H, Spring Kong FM. Effect of radiation fractionation on IDO1 via the NF-κB/COX2 axis in non-small cell lung cancer. Int Immunopharmacol 2023; 124:110956. [PMID: 37751656 DOI: 10.1016/j.intimp.2023.110956] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 03/09/2023] [Revised: 09/13/2023] [Accepted: 09/14/2023] [Indexed: 09/28/2023]
Abstract
Radiotherapy (RT) is the mainstay treatment modality for lung cancer. We recently reported that conventionally fractionated radiotherapy (CRT) with daily fractionation of 2Gy significantly increased the activity of indoleamine 2,3-dioxygenase (IDO1), a known immune checkpoint, which predicted poorer long-term survival in patients with non-small cell lung cancer (NSCLC), while stereotactic body radiotherapy (SBRT) using fractionation size of 10Gy did not increase IDO1 activity and had better survival. Here we hypothesized that the hypofractionated SBRT kind of dose fraction stimulates host antitumor immunity via downregulating IDO1 in which CRT could not. We tested this hypothesis in vitro and in vivo using 10Gyx1 and 2Gyx8 fractionations in the laboratory. The results demonstrated that, although there was an initial downregulation after RT, the expression of IDO1 was ultimately upregulated by both fractionation regimens. The 10Gyx1 regimen had minimum upregulation, while the 2Gyx8 regimen significantly increased in IDO1 expression which was positively correlated with the elevated expressions of p-NF-κB and COX2. Pharmacological inhibition of COX2 abolished RT-induced IDO1 expression. Furthermore, the IDO1 inhibitor, D-1-methyl-tryptophan (D-1MT), exerted RT-related tumor-killing effects in the NSCLC cell lines and mouse models. These findings suggest that, in addition to being an immune suppressor, IDO1 may serve as an adaptive resistance factor in RT. Furthermore, an unappreciated mechanism may exist, where a larger fraction size might be superior to conventional sizes in cancer treatment. This study may provide a rationale for future research in using IDO1 as a biomarker to personalize RT dose fractionation and COX2 inhibitor to decrease radiation immune suppression from CRT.
Collapse
Affiliation(s)
- Yanli Lan
- Key Laboratory of Radiation Oncology of Taizhou, Radiation Oncology Institute of Enze Medical Health Academy, Department of Radiation Oncology, Taizhou Hospital Affiliated to Wenzhou Medical University, Zhejiang Province 317000, China; The Sixth Affiliated Hospital of Wenzhou Medical University, Lishui City People's Hospital, Department of Oncology, Lishui 323000, Zhejiang Province, China
| | - Wenhu Pi
- Key Laboratory of Radiation Oncology of Taizhou, Radiation Oncology Institute of Enze Medical Health Academy, Department of Radiation Oncology, Taizhou Hospital Affiliated to Wenzhou Medical University, Zhejiang Province 317000, China
| | - Zhangjie Zhou
- The Fifth Affiliated Hospital of Wenzhou Medical University, Lishui Municipal Central Hospital, Department of General Medicine, Lishui 323000, Zhejiang Province, China
| | - Yinnan Meng
- Key Laboratory of Radiation Oncology of Taizhou, Radiation Oncology Institute of Enze Medical Health Academy, Department of Radiation Oncology, Taizhou Hospital Affiliated to Wenzhou Medical University, Zhejiang Province 317000, China; Department of Clinical Oncology, Hong Kong University Shenzhen Hospital, Li Ka Shing Faculty of Medicine, the University of Hong Kong, Hong Kong, China
| | - DanMei
- Key Laboratory of Radiation Oncology of Taizhou, Radiation Oncology Institute of Enze Medical Health Academy, Department of Radiation Oncology, Taizhou Hospital Affiliated to Wenzhou Medical University, Zhejiang Province 317000, China
| | - Yixiu Xu
- Key Laboratory of Radiation Oncology of Taizhou, Radiation Oncology Institute of Enze Medical Health Academy, Department of Radiation Oncology, Taizhou Hospital Affiliated to Wenzhou Medical University, Zhejiang Province 317000, China
| | - Xinhang Xia
- Key Laboratory of Radiation Oncology of Taizhou, Radiation Oncology Institute of Enze Medical Health Academy, Department of Radiation Oncology, Taizhou Hospital Affiliated to Wenzhou Medical University, Zhejiang Province 317000, China
| | - WeiWang
- Key Laboratory of Radiation Oncology of Taizhou, Radiation Oncology Institute of Enze Medical Health Academy, Department of Radiation Oncology, Taizhou Hospital Affiliated to Wenzhou Medical University, Zhejiang Province 317000, China
| | - HaiHua Yang
- Key Laboratory of Radiation Oncology of Taizhou, Radiation Oncology Institute of Enze Medical Health Academy, Department of Radiation Oncology, Taizhou Hospital Affiliated to Wenzhou Medical University, Zhejiang Province 317000, China.
| | - Feng-Ming Spring Kong
- Key Laboratory of Radiation Oncology of Taizhou, Radiation Oncology Institute of Enze Medical Health Academy, Department of Radiation Oncology, Taizhou Hospital Affiliated to Wenzhou Medical University, Zhejiang Province 317000, China; Department of Clinical Oncology, Hong Kong University Shenzhen Hospital, Li Ka Shing Faculty of Medicine, the University of Hong Kong, Hong Kong, China.
| |
Collapse
|
|
18
|
Wheeler OPG, Unterholzner L. DNA sensing in cancer: Pro-tumour and anti-tumour functions of cGAS-STING signalling. Essays Biochem 2023; 67:905-918. [PMID: 37534795 PMCID: PMC10539950 DOI: 10.1042/ebc20220241] [Citation(s) in RCA: 3] [Impact Index Per Article: 3.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 03/25/2023] [Revised: 07/11/2023] [Accepted: 07/11/2023] [Indexed: 08/04/2023]
Abstract
The DNA sensor cGAS (cyclic GMP-AMP synthase) and its adaptor protein STING (Stimulator of Interferon Genes) detect the presence of cytosolic DNA as a sign of infection or damage. In cancer cells, this pathway can be activated through persistent DNA damage and chromosomal instability, which results in the formation of micronuclei and the exposure of DNA fragments to the cytosol. DNA damage from radio- or chemotherapy can further activate DNA sensing responses, which may occur in the cancer cells themselves or in stromal and immune cells in the tumour microenvironment (TME). cGAS-STING signalling results in the production of type I interferons, which have been linked to immune cell infiltration in 'hot' tumours that are susceptible to immunosurveillance and immunotherapy approaches. However, recent research has highlighted the complex nature of STING signalling, with tumours having developed mechanisms to evade and hijack this signalling pathway for their own benefit. In this mini-review we will explore how cGAS-STING signalling in different cells in the TME can promote both anti-tumour and pro-tumour responses. This includes the role of type I interferons and the second messenger cGAMP in the TME, and the influence of STING signalling on local immune cell populations. We examine how alternative signalling cascades downstream of STING can promote chronic interferon signalling, the activation of the transcription factor nuclear factor kappa-light-chain-enhancer of activated B cells (NF-κB) and the production of inflammatory cytokines, which can have pro-tumour functions. An in-depth understanding of DNA sensing in different cell contexts will be required to harness the anti-tumour functions of STING signalling.
Collapse
Affiliation(s)
- Otto P G Wheeler
- Division of Biomedical and Life Sciences, Faculty of Health and Medicine, Lancaster University, Lancaster, U.K
| | - Leonie Unterholzner
- Division of Biomedical and Life Sciences, Faculty of Health and Medicine, Lancaster University, Lancaster, U.K
| |
Collapse
|
|
19
|
Yang Y, Wang L, Peugnet-González I, Parada-Venegas D, Dijkstra G, Faber KN. cGAS-STING signaling pathway in intestinal homeostasis and diseases. Front Immunol 2023; 14:1239142. [PMID: 37781354 PMCID: PMC10538549 DOI: 10.3389/fimmu.2023.1239142] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 06/12/2023] [Accepted: 08/18/2023] [Indexed: 10/03/2023] Open
Abstract
The intestinal mucosa is constantly exposed to commensal microbes, opportunistic pathogens, toxins, luminal components and other environmental stimuli. The intestinal mucosa consists of multiple differentiated cellular and extracellular components that form a critical barrier, but is also equipped for efficient absorption of nutrients. Combination of genetic susceptibility and environmental factors are known as critical components involved in the pathogenesis of intestinal diseases. The innate immune system plays a critical role in the recognition and elimination of potential threats by detecting pathogen-associated molecular patterns (PAMPs) and damage-associated molecular patterns (DAMPs). This host defense is facilitated by pattern recognition receptors (PRRs), in which the cyclic GMP-AMP synthase-stimulator of interferon genes (cGAS-STING) pathway has gained attention due to its role in sensing host and foreign double-stranded DNA (dsDNA) as well as cyclic dinucleotides (CDNs) produced by bacteria. Upon binding with dsDNA, cGAS converts ATP and GTP to cyclic GMP-AMP (cGAMP), which binds to STING and activates TANK binding kinase 1 (TBK1) and interferon regulatory factor 3 (IRF3), inducing type I interferon (IFN) and nuclear factor kappa B (NF-κB)-mediated pro-inflammatory cytokines, which have diverse effects on innate and adaptive immune cells and intestinal epithelial cells (IECs). However, opposite perspectives exist regarding the role of the cGAS-STING pathway in different intestinal diseases. Activation of cGAS-STING signaling is associated with worse clinical outcomes in inflammation-associated diseases, while it also plays a critical role in protection against tumorigenesis and certain infections. Therefore, understanding the context-dependent mechanisms of the cGAS-STING pathway in the physiopathology of the intestinal mucosa is crucial for developing therapeutic strategies targeting the cGAS-STING pathway. This review aims to provide insight into recent findings of the protective and detrimental roles of the cGAS-STING pathway in intestinal diseases.
Collapse
Affiliation(s)
- Yuchen Yang
- Department of Gastroenterology and Hepatology, University of Groningen, University Medical Center Groningen, Groningen, Netherlands
| | - Li Wang
- Department of Gastroenterology and Hepatology, University of Groningen, University Medical Center Groningen, Groningen, Netherlands
| | - Ivonne Peugnet-González
- Department of Medical Microbiology and Infection Prevention, University of Groningen, University Medical Center Groningen, Groningen, Netherlands
| | - Daniela Parada-Venegas
- Department of Gastroenterology and Hepatology, University of Groningen, University Medical Center Groningen, Groningen, Netherlands
| | - Gerard Dijkstra
- Department of Gastroenterology and Hepatology, University of Groningen, University Medical Center Groningen, Groningen, Netherlands
| | - Klaas Nico Faber
- Department of Gastroenterology and Hepatology, University of Groningen, University Medical Center Groningen, Groningen, Netherlands
| |
Collapse
|
|
20
|
Liu Y, Pu F. Updated roles of cGAS-STING signaling in autoimmune diseases. Front Immunol 2023; 14:1254915. [PMID: 37781360 PMCID: PMC10538533 DOI: 10.3389/fimmu.2023.1254915] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 07/07/2023] [Accepted: 08/29/2023] [Indexed: 10/03/2023] Open
Abstract
Natural immunity, the first line for the body to defense against the invasion of pathogen, serves as the body's perception of the presence of pathogens depends on nucleic acid recognition mechanisms. The cyclic GMP-AMP synthase-stimulator of the interferon gene (cGAS-STING) signaling pathway is considered an essential pattern recognition and effector pathway in the natural immune system and is mainly responsible for recognizing DNA molecules present in the cytoplasm and activating downstream signaling pathways to generate type I interferons and some other inflammatory factors. STING, a crucial junction protein in the innate immune system, exerts an essential role in host resistance to external pathogen invasion. Also, STING, with the same character of inflammatory molecules, is inseparable from the body's inflammatory response. In particular, when the expression of STING is upregulated or its related signaling pathways are overactivated, the body may develop serious infectious disorders due to the generation of excessive inflammatory responses, non-infectious diseases, and autoimmune diseases. In recent years, accumulating studies indicated that the abnormal activation of the natural immune cGAS-STING signaling pathway modulated by the nucleic acid receptor cGAS closely associated with the development and occurrence of autoimmune diseases (AID). Thereof, to explore an in-depth role of STING and its related signaling pathways in the diseases associated with inflammation may be helpful to provide new avenues for the treatment of these diseases in the clinic. This article reviews the activation process of the cGAS-STING signaling pathways and its related important roles, and therapeutic drugs in AID, aiming to improve our understanding of AID and achieve better diagnosis and treatment of AID.
Collapse
Affiliation(s)
- Ya Liu
- Department of Rheumatology and Immunology, Traditional Chinese and Western Medicine Hospital of Wuhan, Tongji Medical College, Huazhong University of Science and Technology, Wuhan, Hubei, China
- Hubei Key Laboratory of Skin Infection and Immunity, Wuhan No.1 Hospital, Wuhan, Hubei, China
| | - Feifei Pu
- Hubei Key Laboratory of Skin Infection and Immunity, Wuhan No.1 Hospital, Wuhan, Hubei, China
- Department of Orthopedics, Traditional Chinese and Western Medicine Hospital of Wuhan, Tongji Medical College, Huazhong University of Science and Technology, Wuhan, Hubei, China
| |
Collapse
|
|
21
|
Oscherwitz M, Jiminez V, Terhaar H, Yusuf N. Modulation of Skin Cancer by the Stimulator of Interferon Genes. Genes (Basel) 2023; 14:1794. [PMID: 37761934 PMCID: PMC10530941 DOI: 10.3390/genes14091794] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 08/16/2023] [Revised: 09/08/2023] [Accepted: 09/11/2023] [Indexed: 09/29/2023] Open
Abstract
Morbidity and mortality from skin cancer continue to rise domestically and globally, and melanoma and non-melanoma skin cancers are a topic of interest in the dermatology and oncology communities. In this review, we summarize the stimulator of interferon genes (STING) pathway, its specific role in the pathogenesis of DNA damage and skin cancer, and STING-specific therapies that may fight both melanoma and non-melanoma skin (NMSC) cancers. Furthermore, we discuss specific portions of the STING pathway that may be used in addition to previously used therapies to provide a synergistic effect in future oncology treatments and discuss the limitations of current STING-based therapies.
Collapse
Affiliation(s)
- Max Oscherwitz
- Heersink School of Medicine, University of Alabama, Birmingham, AL 35294, USA
| | - Victoria Jiminez
- Heersink School of Medicine, University of Alabama, Birmingham, AL 35294, USA
| | - Hanna Terhaar
- Heersink School of Medicine, University of Alabama, Birmingham, AL 35294, USA
| | - Nabiha Yusuf
- Department of Dermatology, University of Alabama, Birmingham, AL 35294, USA
| |
Collapse
|
|
22
|
Dou Y, Chen R, Liu S, Lee YT, Jing J, Liu X, Ke Y, Wang R, Zhou Y, Huang Y. Optogenetic engineering of STING signaling allows remote immunomodulation to enhance cancer immunotherapy. Nat Commun 2023; 14:5461. [PMID: 37673917 PMCID: PMC10482946 DOI: 10.1038/s41467-023-41164-2] [Citation(s) in RCA: 1] [Impact Index Per Article: 1.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 10/16/2022] [Accepted: 08/22/2023] [Indexed: 09/08/2023] Open
Abstract
The cGAS-STING signaling pathway has emerged as a promising target for immunotherapy development. Here, we introduce a light-sensitive optogenetic device for control of the cGAS/STING signaling to conditionally modulate innate immunity, called 'light-inducible SMOC-like repeats' (LiSmore). We demonstrate that photo-activated LiSmore boosts dendritic cell (DC) maturation and antigen presentation with high spatiotemporal precision. This non-invasive approach photo-sensitizes cytotoxic T lymphocytes to engage tumor antigens, leading to a sustained antitumor immune response. When combined with an immune checkpoint blocker (ICB), LiSmore improves antitumor efficacy in an immunosuppressive lung cancer model that is otherwise unresponsive to conventional ICB treatment. Additionally, LiSmore exhibits an abscopal effect by effectively suppressing tumor growth in a distal site in a bilateral mouse model of melanoma. Collectively, our findings establish the potential of targeted optogenetic activation of the STING signaling pathway for remote immunomodulation in mice.
Collapse
Affiliation(s)
- Yaling Dou
- Institute of Biosciences and Technology, Texas A&M University, Houston, TX, USA
| | - Rui Chen
- Institute of Biosciences and Technology, Texas A&M University, Houston, TX, USA
| | - Siyao Liu
- Institute of Biosciences and Technology, Texas A&M University, Houston, TX, USA
| | - Yi-Tsang Lee
- Institute of Biosciences and Technology, Texas A&M University, Houston, TX, USA
| | - Ji Jing
- Institute of Biosciences and Technology, Texas A&M University, Houston, TX, USA
| | - Xiaoxuan Liu
- Institute of Biosciences and Technology, Texas A&M University, Houston, TX, USA
| | - Yuepeng Ke
- Institute of Biosciences and Technology, Texas A&M University, Houston, TX, USA
| | - Rui Wang
- Institute of Biosciences and Technology, Texas A&M University, Houston, TX, USA
| | - Yubin Zhou
- Institute of Biosciences and Technology, Texas A&M University, Houston, TX, USA.
- Department of Translational Medical Sciences, School of Medicine, Texas A&M University, Houston, TX, 77030, USA.
| | - Yun Huang
- Institute of Biosciences and Technology, Texas A&M University, Houston, TX, USA.
- Department of Translational Medical Sciences, School of Medicine, Texas A&M University, Houston, TX, 77030, USA.
| |
Collapse
|
|
23
|
Yang C, Liang Y, Liu N, Sun M. Role of the cGAS-STING pathway in radiotherapy for non-small cell lung cancer. Radiat Oncol 2023; 18:145. [PMID: 37667279 PMCID: PMC10478265 DOI: 10.1186/s13014-023-02335-z] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 10/13/2022] [Accepted: 08/22/2023] [Indexed: 09/06/2023] Open
Abstract
One of the most important therapeutic interventions for non-small cell lung cancer is radiotherapy. Ionizing radiation (IR) is classified by traditional radiobiology principles as a direct cytocidal therapeutic agent against cancer, although there is growing recognition of other antitumor immunological responses induced by this modality. The most effective therapeutic combinations to harness radiation-generated antitumor immunity and enhance treatment results for malignancies resistant to existing radiotherapy regimens could be determined by a more sophisticated understanding of the immunological pathways created by radiation. Innate immune signaling is triggered by the activation of cGAS-STING, and this promotes adaptive immune responses to help fight cancer. This identifies a molecular mechanism radiation can use to trigger antitumor immune responses by bridging the DNA-damaging ability of IR with the activation of CD8 + cytotoxic T cell-mediated killing of tumors. We also discuss radiotherapy-related parameters that affect cGAS-STING signaling, negative consequences of cGAS-STING activation, and intriguing treatment options being tested in conjunction with IR to support immune activation by activating STING-signaling. Improved therapeutic outcomes will result from a better understanding of how IR promotes cGAS-STING signaling in immune-based treatment regimens that maximize radiotherapy's anticancer effectiveness.
Collapse
Affiliation(s)
- Chunsheng Yang
- Department of Oncology, Central Hospital Affiliated to Shandong First Medical University, Jinan City, China
| | - Yan Liang
- Department of Radiation, The Second Affiliated Hospital of Xingtai Medical College, Xing Tai Shi, China
| | - Ning Liu
- Department of Oncology, Central Hospital Affiliated to Shandong First Medical University, Jinan City, China
| | - Meili Sun
- Department of Oncology, Central Hospital Affiliated to Shandong First Medical University, Jinan City, China.
| |
Collapse
|
|
24
|
Qin Z, Liu H, Sheng Q, Dan J, Wu X, Li H, Wang L, Zhang S, Yuan C, Yuan H, Wang H, Zhou R, Luo Y, Xie X. Mutant p53 leads to low-grade IFN-I-induced inflammation and impairs cGAS-STING signalling in mice. Eur J Immunol 2023; 53:e2250211. [PMID: 37377275 DOI: 10.1002/eji.202250211] [Citation(s) in RCA: 1] [Impact Index Per Article: 1.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 10/19/2022] [Revised: 05/09/2023] [Accepted: 05/31/2023] [Indexed: 06/29/2023]
Abstract
Type I interferons (IFN-Is) are a class of proinflammatory cytokines produced in response to viruses and environmental stimulations, resulting in chronic inflammation and even carcinogenesis. However, the connection between IFN-I and p53 mutation is poorly understood. Here, we investigated IFN-I status in the context of mutant p53 (p53N236S , p53S). We observed significant cytosolic double-stranded DNA (dsDNA) derived from nuclear heterochromatin in p53S cells, along with an increased expression of IFN-stimulated genes. Further study revealed that p53S promoted cyclic GMP-AMP synthase (cGAS) and IFN-regulatory factor 9 (IRF9) expression, thus activating the IFN-I pathway. However, p53S/S mice were more susceptible to herpes simplex virus 1 infection, and the cGAS-stimulator of IFN genes (STING) pathway showed a decline trend in p53S cells in response to poly(dA:dT) accompanied with decreased IFN-β and IFN-stimulated genes, whereas the IRF9 increased in response to IFN-β stimulation. Our results illustrated the p53S mutation leads to low-grade IFN-I-induced inflammation via consistent low activation of the cGAS-STING-IFN-I axis, and STAT1-IRF9 pathway, therefore, impairs the protective cGAS-STING signalling and IFN-I response encountered with exogenous DNA attack. These results suggested the dual molecular mechanisms of p53S mutation in inflammation regulation. Our results could be helping in further understanding of mutant p53 function in chronic inflammation and provide information for developing new therapeutic strategies for chronic inflammatory diseases or cancer.
Collapse
Affiliation(s)
- Ziyi Qin
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| | - Huan Liu
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| | - Qihuan Sheng
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| | - Juhua Dan
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| | - Xiaoming Wu
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| | - Hao Li
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| | - Lulin Wang
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| | - Shuojie Zhang
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| | - Chao Yuan
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| | - Hongjun Yuan
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| | - Hui Wang
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| | - Ruoyu Zhou
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| | - Ying Luo
- Guizhou Provincial Key Laboratory of Pathogenesis & Drug Development on Common Chronic Diseases, School of Basic Medicine, Guizhou Medical University, Guiyang, Guizhou, China
| | - Xiaoli Xie
- Molecular Genetics Laboratory of Aging and Tumor, Medical School, Kunming University of Science and Technology, Kunming, Yunnan, China
| |
Collapse
|
|
25
|
Zou Y, Zhang M, Zhou J. Recent trends in STING modulators: Structures, mechanisms, and therapeutic potential. Drug Discov Today 2023; 28:103694. [PMID: 37393985 DOI: 10.1016/j.drudis.2023.103694] [Citation(s) in RCA: 2] [Impact Index Per Article: 2.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/17/2023] [Revised: 06/05/2023] [Accepted: 06/26/2023] [Indexed: 07/04/2023]
Abstract
The cyclic GMP-AMP synthase stimulator (cGAS)-stimulator of interferon gene (STING) signaling pathway has an integral role in the host immune response through DNA sensing followed by inducing a robust innate immune defense program. STING has become a promising therapeutic target associated with multiple diseases, including various inflammatory diseases, cancer, and infectious diseases, among others. Thus, modulators of STING are regarded as emerging therapeutic agents. Recent progress has been made in STING research, including recently identified STING-mediated regulatory pathways, the development of a new STING modulator, and the new association of STING with disease. In this review, we focus on recent trends in the development of STING modulators, including structures, mechanisms, and clinical application.
Collapse
Affiliation(s)
- Yan Zou
- Key Laboratory of the Ministry of Education for Advanced Catalysis Materials, Department of Chemistry, Zhejiang Normal University, 688 Yingbin Road, Jinhua 321004, China; Drug Development and Innovation Center, College of Chemistry and Life Sciences, Zhejiang Normal University, 688 Yingbin Road, Jinhua 321004, China
| | - Min Zhang
- Key Laboratory of the Ministry of Education for Advanced Catalysis Materials, Department of Chemistry, Zhejiang Normal University, 688 Yingbin Road, Jinhua 321004, China; Drug Development and Innovation Center, College of Chemistry and Life Sciences, Zhejiang Normal University, 688 Yingbin Road, Jinhua 321004, China
| | - Jinming Zhou
- Key Laboratory of the Ministry of Education for Advanced Catalysis Materials, Department of Chemistry, Zhejiang Normal University, 688 Yingbin Road, Jinhua 321004, China; Drug Development and Innovation Center, College of Chemistry and Life Sciences, Zhejiang Normal University, 688 Yingbin Road, Jinhua 321004, China.
| |
Collapse
|
|
26
|
Zhou J, Zhuang Z, Li J, Feng Z. Significance of the cGAS-STING Pathway in Health and Disease. Int J Mol Sci 2023; 24:13316. [PMID: 37686127 PMCID: PMC10487967 DOI: 10.3390/ijms241713316] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 06/30/2023] [Revised: 08/18/2023] [Accepted: 08/22/2023] [Indexed: 09/10/2023] Open
Abstract
The cyclic GMP-AMP synthase (cGAS)-stimulator of interferon genes (STING) pathway plays a significant role in health and disease. In this pathway, cGAS, one of the major cytosolic DNA sensors in mammalian cells, regulates innate immunity and the STING-dependent production of pro-inflammatory cytokines, including type-I interferon. Moreover, the cGAS-STING pathway is integral to other cellular processes, such as cell death, cell senescence, and autophagy. Activation of the cGAS-STING pathway by "self" DNA is also attributed to various infectious diseases and autoimmune or inflammatory conditions. In addition, the cGAS-STING pathway activation functions as a link between innate and adaptive immunity, leading to the inhibition or facilitation of tumorigenesis; therefore, research targeting this pathway can provide novel clues for clinical applications to treat infectious, inflammatory, and autoimmune diseases and even cancer. In this review, we focus on the cGAS-STING pathway and its corresponding cellular and molecular mechanisms in health and disease.
Collapse
Affiliation(s)
- Jinglin Zhou
- Fujian Key Laboratory of Innate Immune Biology, Biomedical Research Center of South China, College of Life Science, Fujian Normal University Qishan Campus, Fuzhou 350117, China
| | - Zhan Zhuang
- Key Laboratory of College of First Clinical Medicine, College of First Clinical Medicine, Fujian Medical University, Taijiang Campus, Fuzhou 350001, China
| | - Jiamian Li
- Key Laboratory of College of First Clinical Medicine, College of First Clinical Medicine, Fujian Medical University, Taijiang Campus, Fuzhou 350001, China
| | - Zhihua Feng
- Fujian Key Laboratory of Innate Immune Biology, Biomedical Research Center of South China, College of Life Science, Fujian Normal University Qishan Campus, Fuzhou 350117, China
| |
Collapse
|
|
27
|
Lewicky JD, Martel AL, Gupta MR, Roy R, Rodriguez GM, Vanderhyden BC, Le HT. Conventional DNA-Damaging Cancer Therapies and Emerging cGAS-STING Activation: A Review and Perspectives Regarding Immunotherapeutic Potential. Cancers (Basel) 2023; 15:4127. [PMID: 37627155 PMCID: PMC10453198 DOI: 10.3390/cancers15164127] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 07/11/2023] [Revised: 08/10/2023] [Accepted: 08/11/2023] [Indexed: 08/27/2023] Open
Abstract
Many traditional cancer treatments such as radiation and chemotherapy are known to induce cellular DNA damage as part of their cytotoxic activity. The cGAS-STING signaling axis, a key member of the DNA damage response that acts as a sensor of foreign or aberrant cytosolic DNA, is helping to rationalize the DNA-damaging activity of these treatments and their emerging immunostimulatory capacity. Moreover, cGAS-STING, which is attracting considerable attention for its ability to promote antitumor immune responses, may fundamentally be able to address many of the barriers limiting the success of cancer immunotherapy strategies, including the immunosuppressive tumor microenvironment. Herein, we review the traditional cancer therapies that have been linked with cGAS-STING activation, highlighting their targets with respect to their role and function in the DNA damage response. As part of the review, an emerging "chemoimmunotherapy" concept whereby DNA-damaging agents are used for the indirect activation of STING is discussed as an alternative to the direct molecular agonism strategies that are in development, but have yet to achieve clinical approval. The potential of this approach to address some of the inherent and emerging limitations of cGAS-STING signaling in cancer immunotherapy is also discussed. Ultimately, it is becoming clear that in order to successfully employ the immunotherapeutic potential of the cGAS-STING axis, a balance between its contrasting antitumor and protumor/inflammatory activities will need to be achieved.
Collapse
Affiliation(s)
- Jordan D. Lewicky
- Health Sciences North Research Institute, 56 Walford Road, Sudbury, ON P3E 2H2, Canada; (J.D.L.); (A.L.M.)
| | - Alexandrine L. Martel
- Health Sciences North Research Institute, 56 Walford Road, Sudbury, ON P3E 2H2, Canada; (J.D.L.); (A.L.M.)
| | - Mukul Raj Gupta
- Glycosciences and Nanomaterial Laboratory, Université du Québec à Montréal, Succ. Centre-Ville, Montréal, QC H3C 3P8, Canada; (M.R.G.); (R.R.)
| | - René Roy
- Glycosciences and Nanomaterial Laboratory, Université du Québec à Montréal, Succ. Centre-Ville, Montréal, QC H3C 3P8, Canada; (M.R.G.); (R.R.)
| | - Galaxia M. Rodriguez
- Cancer Therapeutics Program, Ottawa Hospital Research Institute, 501 Smyth Rd., Ottawa, ON K1H 8L6, Canada; (G.M.R.); (B.C.V.)
- Department of Cellular and Molecular Medicine, University of Ottawa, 451 Smyth Rd., Ottawa, ON K1H 8M5, Canada
| | - Barbara C. Vanderhyden
- Cancer Therapeutics Program, Ottawa Hospital Research Institute, 501 Smyth Rd., Ottawa, ON K1H 8L6, Canada; (G.M.R.); (B.C.V.)
- Department of Cellular and Molecular Medicine, University of Ottawa, 451 Smyth Rd., Ottawa, ON K1H 8M5, Canada
| | - Hoang-Thanh Le
- Health Sciences North Research Institute, 56 Walford Road, Sudbury, ON P3E 2H2, Canada; (J.D.L.); (A.L.M.)
- Medicinal Sciences Division, NOSM University, 935 Ramsey Lake Road, Sudbury, ON P3E 2C6, Canada
- School of Natural Sciences, Laurentian University, 935 Ramsey Lake Road, Sudbury, ON P3E 2C6, Canada
| |
Collapse
|
|
28
|
Alshebremi M, Tomchuck SL, Myers JT, Kingsley DT, Eid S, Abiff M, Bonner M, Saab ST, Choi SH, Huang AYC. Functional tumor cell-intrinsic STING, not host STING, drives local and systemic antitumor immunity and therapy efficacy following cryoablation. J Immunother Cancer 2023; 11:e006608. [PMID: 37553183 PMCID: PMC10414127 DOI: 10.1136/jitc-2022-006608] [Citation(s) in RCA: 1] [Impact Index Per Article: 1.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Accepted: 07/12/2023] [Indexed: 08/10/2023] Open
Abstract
BACKGROUND Despite its potential utility in delivering direct tumor killing and in situ whole-cell tumor vaccination, tumor cryoablation produces highly variable and unpredictable clinical response, limiting its clinical utility. The mechanism(s) driving cryoablation-induced local antitumor immunity and the associated abscopal effect is not well understood. METHODS The aim of this study was to identify and explore a mechanism of action by which cryoablation enhances the therapeutic efficacy in metastatic tumor models. We used the subcutaneous mouse model of the rhabdomyosarcoma (RMS) cell lines RMS 76-9STINGwt or RMS 76-9STING-/-, along with other murine tumor models, in C57BL/6 or STING-/- (TMEM173-/- ) mice to evaluate local tumor changes, lung metastasis, abscopal effect on distant tumors, and immune cell dynamics in the tumor microenvironment (TME). RESULTS The results show that cryoablation efficacy is dependent on both adaptive immunity and the STING signaling pathway. Contrary to current literature dictating an essential role of host-derived STING activation as a driver of antitumor immunity in vivo, we show that local tumor control, lung metastasis, and the abscopal effect on distant tumor are all critically dependent on a functioning tumor cell-intrinsic STING signaling pathway, which induces inflammatory chemokine and cytokine responses in the cryoablated TME. This reliance extends beyond cryoablation to include intratumoral STING agonist therapy. Additionally, surveys of gene expression databases and tissue microarrays of clinical tumor samples revealed a wide spectrum of expressions among STING-related signaling components. CONCLUSIONS Tumor cell-intrinsic STING pathway is a critical component underlying the effectiveness of cryoablation and suggests that expression of STING-related signaling components may serve as a potential therapy response biomarker. Our data also highlight an urgent need to further characterize tumor cell-intrinsic STING pathways and the associated downstream inflammatory response evoked by cryoablation and other STING-dependent therapy approaches.
Collapse
Affiliation(s)
- Mohammad Alshebremi
- Department of Pathology, Case Western Reserve University School of Medicine, Cleveland, Ohio, USA
- Department of Medical Laboratories, College of Applied Medical Sciences, Qassim University, Buraydah, Saudi Arabia
| | - Suzanne L Tomchuck
- Department of Pediatrics, Case Western Reserve University School of Medicine, Cleveland, Ohio, USA
| | - Jay T Myers
- Department of Pediatrics, Case Western Reserve University School of Medicine, Cleveland, Ohio, USA
| | - Daniel T Kingsley
- Department of Pathology, Case Western Reserve University School of Medicine, Cleveland, Ohio, USA
| | - Saada Eid
- Department of Pediatrics, Case Western Reserve University School of Medicine, Cleveland, Ohio, USA
| | - Muta Abiff
- Department of Pathology, Case Western Reserve University School of Medicine, Cleveland, Ohio, USA
| | - Melissa Bonner
- Department of Pathology, Case Western Reserve University School of Medicine, Cleveland, Ohio, USA
| | - Shahrazad T Saab
- Department of Pathology, University Hospitals Cleveland Medical Center, Cleveland, Ohio, USA
| | - Sung Hee Choi
- Department of Pediatrics, Case Western Reserve University School of Medicine, Cleveland, Ohio, USA
| | - Alex Yee-Chen Huang
- Department of Pathology, Case Western Reserve University School of Medicine, Cleveland, Ohio, USA
- Department of Pediatrics, Case Western Reserve University School of Medicine, Cleveland, Ohio, USA
- Center for Pediatric Immunotherapy, Angie Fowler AYA Cancer Institute, UH Rainbow Babies & Children's Hospital, Cleveland, Ohio, USA
| |
Collapse
|
|
29
|
Deng X, Qing Y, Chen J. Targeting YTHDF2/MDSCs to improve radiotherapy. Cell Chem Biol 2023; 30:703-705. [PMID: 37478827 DOI: 10.1016/j.chembiol.2023.06.024] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 06/23/2023] [Revised: 06/26/2023] [Accepted: 06/27/2023] [Indexed: 07/23/2023]
Abstract
Immunosuppression contributes to tumor-radiotherapy failure, but the mechanism remains elusive. Wang et al.1 reported that ionizing radiation (IR) induces YTHDF2 expression in myeloid-derived suppressor cells (MDSCs) via an IR-YTHDF2-NF-κB circuit, which contributes to MDSC expansion/migration and treatment failure. Genetic depletion or pharmacological inhibition of YTHDF2 overcomes immunosuppression and improves radiotherapy.
Collapse
Affiliation(s)
- Xiaolan Deng
- Department of Systems Biology, Beckman Research Institute of City of Hope, Monrovia, CA 91016, USA
| | - Ying Qing
- Department of Systems Biology, Beckman Research Institute of City of Hope, Monrovia, CA 91016, USA
| | - Jianjun Chen
- Department of Systems Biology, Beckman Research Institute of City of Hope, Monrovia, CA 91016, USA; City of Hope Comprehensive Cancer Center, City of Hope, Duarte, CA 91010, USA; Gehr Family Center for Leukemia Research & City of Hope Comprehensive Cancer Center, City of Hope, Duarte, CA 91010, USA.
| |
Collapse
|
|
30
|
Wang L, Dou X, Chen S, Yu X, Huang X, Zhang L, Chen Y, Wang J, Yang K, Bugno J, Pitroda S, Ding X, Piffko A, Si W, Chen C, Jiang H, Zhou B, Chmura SJ, Luo C, Liang HL, He C, Weichselbaum RR. YTHDF2 inhibition potentiates radiotherapy antitumor efficacy. Cancer Cell 2023; 41:1294-1308.e8. [PMID: 37236197 PMCID: PMC10524856 DOI: 10.1016/j.ccell.2023.04.019] [Citation(s) in RCA: 14] [Impact Index Per Article: 14.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Submit a Manuscript] [Subscribe] [Scholar Register] [Received: 08/30/2022] [Revised: 12/23/2022] [Accepted: 04/28/2023] [Indexed: 05/28/2023]
Abstract
RNA N6-methyladenosine (m6A) modification is implicated in cancer progression. However, the impact of m6A on the antitumor effects of radiotherapy and the related mechanisms are unknown. Here we show that ionizing radiation (IR) induces immunosuppressive myeloid-derived suppressor cell (MDSC) expansion and YTHDF2 expression in both murine models and humans. Following IR, loss of Ythdf2 in myeloid cells augments antitumor immunity and overcomes tumor radioresistance by altering MDSC differentiation and inhibiting MDSC infiltration and suppressive function. The remodeling of the landscape of MDSC populations by local IR is reversed by Ythdf2 deficiency. IR-induced YTHDF2 expression relies on NF-κB signaling; YTHDF2 in turn leads to NF-κB activation by directly binding and degrading transcripts encoding negative regulators of NF-κB signaling, resulting in an IR-YTHDF2-NF-κB circuit. Pharmacological inhibition of YTHDF2 overcomes MDSC-induced immunosuppression and improves combined IR and/or anti-PD-L1 treatment. Thus, YTHDF2 is a promising target to improve radiotherapy (RT) and RT/immunotherapy combinations.
Collapse
Affiliation(s)
- Liangliang Wang
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA
| | - Xiaoyang Dou
- Department of Chemistry, Department of Biochemistry and Molecular Biology, and Institute for Biophysical Dynamics, The University of Chicago, Chicago, IL 60637, USA; Howard Hughes Medical Institute, University of Chicago, Chicago, IL 60637, USA
| | - Shijie Chen
- State Key Laboratory of Drug Research, Shanghai Institute of Materia Medica, Chinese Academy of Sciences, Shanghai 201203, China
| | - Xianbin Yu
- Department of Chemistry, Department of Biochemistry and Molecular Biology, and Institute for Biophysical Dynamics, The University of Chicago, Chicago, IL 60637, USA; Howard Hughes Medical Institute, University of Chicago, Chicago, IL 60637, USA
| | - Xiaona Huang
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA
| | - Linda Zhang
- Department of Chemistry, Department of Biochemistry and Molecular Biology, and Institute for Biophysical Dynamics, The University of Chicago, Chicago, IL 60637, USA; Howard Hughes Medical Institute, University of Chicago, Chicago, IL 60637, USA
| | - Yantao Chen
- State Key Laboratory of Drug Research, Shanghai Institute of Materia Medica, Chinese Academy of Sciences, Shanghai 201203, China
| | - Jiaai Wang
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA
| | - Kaiting Yang
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA
| | - Jason Bugno
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA; The Committee on Clinical Pharmacology and Pharmacogenomics, University of Chicago, Chicago, IL 600637, USA
| | - Sean Pitroda
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA
| | - Xingchen Ding
- Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, Jinan 250117, China
| | - Andras Piffko
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA; Department of Neurosurgery, University Medical Center Hamburg-Eppendorf, Hamburg 20246, Germany
| | - Wei Si
- State Key Laboratory of Animal Nutrition, Institute of Animal Science, Chinese Academy of Agricultural Sciences, Beijing 100193, China
| | - Chao Chen
- State Key Laboratory of Drug Research, Shanghai Institute of Materia Medica, Chinese Academy of Sciences, Shanghai 201203, China
| | - Hualiang Jiang
- State Key Laboratory of Drug Research, Shanghai Institute of Materia Medica, Chinese Academy of Sciences, Shanghai 201203, China
| | - Bing Zhou
- State Key Laboratory of Drug Research, Shanghai Institute of Materia Medica, Chinese Academy of Sciences, Shanghai 201203, China
| | - Steven J Chmura
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA
| | - Cheng Luo
- State Key Laboratory of Drug Research, Shanghai Institute of Materia Medica, Chinese Academy of Sciences, Shanghai 201203, China; Zhongshan Institute for Drug Discovery, Shanghai Institute of Materia Medica, Chinese Academy of Sciences, Zhongshan 528437, China.
| | - Hua Laura Liang
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA.
| | - Chuan He
- Department of Chemistry, Department of Biochemistry and Molecular Biology, and Institute for Biophysical Dynamics, The University of Chicago, Chicago, IL 60637, USA; Howard Hughes Medical Institute, University of Chicago, Chicago, IL 60637, USA; Department of Biochemistry and Molecular Biology, University of Chicago, Chicago, IL 60637, USA.
| | - Ralph R Weichselbaum
- Department of Radiation and Cellular Oncology, University of Chicago, Chicago, IL 60637, USA; Ludwig Center for Metastasis Research, University of Chicago, Chicago, IL 60637, USA.
| |
Collapse
|
|
31
|
Liu Y, Fei Y, Wang X, Yang B, Li M, Luo Z. Biomaterial-enabled therapeutic modulation of cGAS-STING signaling for enhancing antitumor immunity. Mol Ther 2023; 31:1938-1959. [PMID: 37002605 PMCID: PMC10362396 DOI: 10.1016/j.ymthe.2023.03.026] [Citation(s) in RCA: 2] [Impact Index Per Article: 2.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 12/06/2022] [Revised: 03/07/2023] [Accepted: 03/23/2023] [Indexed: 04/03/2023] Open
Abstract
cGAS-STING signaling is a central component in the therapeutic action of most existing cancer therapies. The accumulated knowledge of tumor immunoregulatory network in recent years has spurred the development of cGAS-STING agonists for tumor treatment as an effective immunotherapeutic strategy. However, the clinical translation of these agonists is thus far unsatisfactory because of the low immunostimulatory efficacy and unrestricted side effects under clinically relevant conditions. Interestingly, the rational integration of biomaterial technology offers a promising approach to overcome these limitations for more effective and safer cGAS-STING-mediated tumor therapy. Herein, we first outline the cGAS-STING signaling axis and generally discuss its association with tumors. We then symmetrically summarize the recent progress in those biomaterial-based cGAS-STING agonism strategies to generate robust antitumor immunity, categorized by the chemical nature of those cGAS-STING stimulants and carrier substrates. Finally, a perspective is provided to discuss the existing challenges and potential opportunities in cGAS-STING modulation for tumor therapy.
Collapse
Affiliation(s)
- Yingqi Liu
- School of Life Science, Chongqing University, Chongqing 400044, P. R. China
| | - Yang Fei
- School of Life Science, Chongqing University, Chongqing 400044, P. R. China
| | - Xuan Wang
- School of Life Science, Chongqing University, Chongqing 400044, P. R. China
| | - Bingbing Yang
- School of Life Science, Chongqing University, Chongqing 400044, P. R. China
| | - Menghuan Li
- School of Life Science, Chongqing University, Chongqing 400044, P. R. China.
| | - Zhong Luo
- School of Life Science, Chongqing University, Chongqing 400044, P. R. China.
| |
Collapse
|
|
32
|
Chauvin SD, Stinson WA, Platt DJ, Poddar S, Miner JJ. Regulation of cGAS and STING signaling during inflammation and infection. J Biol Chem 2023; 299:104866. [PMID: 37247757 PMCID: PMC10316007 DOI: 10.1016/j.jbc.2023.104866] [Citation(s) in RCA: 2] [Impact Index Per Article: 2.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 10/04/2021] [Revised: 05/16/2023] [Accepted: 05/17/2023] [Indexed: 05/31/2023] Open
Abstract
Stimulator of interferon genes (STING) is a sensor of cyclic dinucleotides including cyclic GMP-AMP, which is produced by cyclic GMP-AMP synthase (cGAS) in response to cytosolic DNA. The cGAS-STING signaling pathway regulates both innate and adaptive immune responses, as well as fundamental cellular functions such as autophagy, senescence, and apoptosis. Mutations leading to constitutive activation of STING cause devastating human diseases. Thus, the cGAS-STING pathway is of great interest because of its role in diverse cellular processes and because of the potential therapeutic implications of targeting cGAS and STING. Here, we review molecular and cellular mechanisms of STING signaling, and we propose a framework for understanding the immunological and other cellular functions of STING in the context of disease.
Collapse
Affiliation(s)
- Samuel D Chauvin
- Departments of Medicine and Microbiology, University of Pennsylvania Perelman School of Medicine, Philadelphia, Pennsylvania, USA
| | - W Alexander Stinson
- Departments of Pathology and Immunology, Washington University School of Medicine, Saint Louis, Missouri, USA
| | - Derek J Platt
- Department Molecular Microbiology, Washington University School of Medicine, Saint Louis, Missouri, USA
| | - Subhajit Poddar
- Departments of Medicine and Microbiology, University of Pennsylvania Perelman School of Medicine, Philadelphia, Pennsylvania, USA
| | - Jonathan J Miner
- Departments of Medicine and Microbiology, University of Pennsylvania Perelman School of Medicine, Philadelphia, Pennsylvania, USA; Departments of Pathology and Immunology, Washington University School of Medicine, Saint Louis, Missouri, USA; Department Molecular Microbiology, Washington University School of Medicine, Saint Louis, Missouri, USA; Department of Medicine, Washington University School of Medicine, Saint Louis, Missouri, USA.
| |
Collapse
|
|
33
|
Zhu M, Tang X, Zhu Z, Gong Z, Tang W, Hu Y, Cheng C, Wang H, Sarwar A, Chen Y, Liu F, Huo J, Wang X, Zhang Y. STING activation in macrophages by vanillic acid exhibits antineoplastic potential. Biochem Pharmacol 2023; 213:115618. [PMID: 37211172 DOI: 10.1016/j.bcp.2023.115618] [Citation(s) in RCA: 6] [Impact Index Per Article: 6.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 02/24/2023] [Revised: 05/12/2023] [Accepted: 05/15/2023] [Indexed: 05/23/2023]
Abstract
The host stimulator of interferon genes (STING) signaling pathway is a major innate immune sensing pathway, and the stimulation of this pathway within antigen-presenting cells shows promise in targeting immune-suppressed tumors. Macrophages resident in tumors exhibit anti-inflammatory properties and enhance tumor growth and development. Polarizing such macrophages towards a pro-inflammatory phenotype is an effective strategy for tumor suppression. In the present study, we observed that the STING pathway was inactivated in breast and lung carcinomas, and a positive correlation existed between STING and macrophage markers in these tumors. We found that vanillic acid (VA) could stimulate the STING/TBK1/IRF3 pathway. VA mediated the production of type I IFN and promoted macrophage polarization into the M1 phenotype; this activity was dependent on STING activation. A direct-contact co-culture model and a transwell co-culture model revealed that macrophages with VA-induced STING activation exhibited anti-proliferative effects on SKBR3 and H1299 cells, although a STING antagonist and M2 macrophage-related cytokines alleviated this anti-proliferative effect. Further investigation indicated that phagocytosis and apoptosis-inducing effects were the major mediators of the anti-tumor effect of VA-treated macrophages. Mechanistically, VA promoted the polarization of macrophages to a M1 phenotype via IL-6R/JAK signaling, resulting in enhanced phagocytosis and apoptosis-induction effects. Additionally, STING activation-induced IFNβ production also participated in the apoptosis mediated by VA-treated macrophage in SKBR3 and H1299 cells. Mouse models with 4 T1 tumors confirmed the anti-tumor properties of VA in vivo and revealed the infiltration of VA-induced cytotoxic T cells into the tumors. These data suggest that VA is an effective agonist of STING and provides a new perspective for cancer immunotherapy.
Collapse
Affiliation(s)
- Man Zhu
- School of Pharmacy, Health Science Center, Xi'an Jiaotong University, No. 76, Yanta Weststreet, #54, Xi'an, Shaanxi Province 710061, China; State Key Laboratory of Shaanxi for Natural Medicines Research and Engineering, Xi'an Jiaotong University, Xi'an 710061, China
| | - Xiaoyu Tang
- School of Pharmacy, Health Science Center, Xi'an Jiaotong University, No. 76, Yanta Weststreet, #54, Xi'an, Shaanxi Province 710061, China; State Key Laboratory of Shaanxi for Natural Medicines Research and Engineering, Xi'an Jiaotong University, Xi'an 710061, China
| | - Zeren Zhu
- School of Pharmacy, Health Science Center, Xi'an Jiaotong University, No. 76, Yanta Weststreet, #54, Xi'an, Shaanxi Province 710061, China; State Key Laboratory of Shaanxi for Natural Medicines Research and Engineering, Xi'an Jiaotong University, Xi'an 710061, China
| | - Zhengyan Gong
- School of Pharmacy, Health Science Center, Xi'an Jiaotong University, No. 76, Yanta Weststreet, #54, Xi'an, Shaanxi Province 710061, China; State Key Laboratory of Shaanxi for Natural Medicines Research and Engineering, Xi'an Jiaotong University, Xi'an 710061, China
| | - Wenjuan Tang
- School of Pharmacy, Health Science Center, Xi'an Jiaotong University, No. 76, Yanta Weststreet, #54, Xi'an, Shaanxi Province 710061, China; State Key Laboratory of Shaanxi for Natural Medicines Research and Engineering, Xi'an Jiaotong University, Xi'an 710061, China
| | - Yu Hu
- School of Pharmacy, Health Science Center, Xi'an Jiaotong University, No. 76, Yanta Weststreet, #54, Xi'an, Shaanxi Province 710061, China; State Key Laboratory of Shaanxi for Natural Medicines Research and Engineering, Xi'an Jiaotong University, Xi'an 710061, China
| | - Cheng Cheng
- School of Pharmacy, Health Science Center, Xi'an Jiaotong University, No. 76, Yanta Weststreet, #54, Xi'an, Shaanxi Province 710061, China; State Key Laboratory of Shaanxi for Natural Medicines Research and Engineering, Xi'an Jiaotong University, Xi'an 710061, China
| | - Hongying Wang
- School of Pharmacy, Health Science Center, Xi'an Jiaotong University, No. 76, Yanta Weststreet, #54, Xi'an, Shaanxi Province 710061, China; State Key Laboratory of Shaanxi for Natural Medicines Research and Engineering, Xi'an Jiaotong University, Xi'an 710061, China
| | - Ammar Sarwar
- School of Pharmacy, Health Science Center, Xi'an Jiaotong University, No. 76, Yanta Weststreet, #54, Xi'an, Shaanxi Province 710061, China; State Key Laboratory of Shaanxi for Natural Medicines Research and Engineering, Xi'an Jiaotong University, Xi'an 710061, China
| | - Yanbin Chen
- Shaanxi Institute of International Trade & Commerce, Xianyang 712046, China; Shaanxi Buchang Pharmaceutical Co. Ltd, Xi'an 710075, China
| | - Feng Liu
- Shaanxi Institute of International Trade & Commerce, Xianyang 712046, China; Shaanxi Buchang Pharmaceutical Co. Ltd, Xi'an 710075, China
| | - Jian Huo
- School of Pharmacy, Health Science Center, Xi'an Jiaotong University, No. 76, Yanta Weststreet, #54, Xi'an, Shaanxi Province 710061, China; State Key Laboratory of Shaanxi for Natural Medicines Research and Engineering, Xi'an Jiaotong University, Xi'an 710061, China
| | - Xuemei Wang
- School of Pharmacy, Health Science Center, Xi'an Jiaotong University, No. 76, Yanta Weststreet, #54, Xi'an, Shaanxi Province 710061, China; State Key Laboratory of Shaanxi for Natural Medicines Research and Engineering, Xi'an Jiaotong University, Xi'an 710061, China
| | - Yanmin Zhang
- School of Pharmacy, Health Science Center, Xi'an Jiaotong University, No. 76, Yanta Weststreet, #54, Xi'an, Shaanxi Province 710061, China; State Key Laboratory of Shaanxi for Natural Medicines Research and Engineering, Xi'an Jiaotong University, Xi'an 710061, China.
| |
Collapse
|
|
34
|
Abstract
Myeloid immune cells (MICs) are potent innate immune cells serving as first responders to invading pathogens and internal changes to cellular homeostasis. Cancer is a stage of altered cellular homeostasis that can originate in response to different pathogens, chemical carcinogens, and internal genetic/epigenetic changes. MICs express several pattern recognition receptors (PRRs) on their membranes, cytosol, and organelles, recognizing systemic, tissue, and organ-specific altered homeostasis. cGAS/STING signaling is a cytosolic PRR system for identifying cytosolic double-stranded DNA (dsDNA) in a sequence-independent but size-dependent manner. The longer the cytosolic dsDNA size, the stronger the cGAS/STING signaling activation with increased type 1 interferon (IFN) and NF-κB-dependent cytokines and chemokines' generation. The present article discusses tumor-supportive changes occurring in the tumor microenvironment (TME) or tumor immune microenvironment (TIME) MICs, specifically emphasizing cGAS/STING signaling-dependent alteration. The article further discusses utilizing MIC-specific cGAS/STING signaling modulation as critical tumor immunotherapy to alter TIME.
Collapse
Affiliation(s)
- Vijay Kumar
- Department of Interdisciplinary Oncology, Stanley S. Scott Cancer Center, School of Medicine, Louisiana State University Health Science Center (LSUHSC), 1700 Tulane Avenue, New Orleans, LA, 70012, USA.
| | - Caitlin Bauer
- Department of Interdisciplinary Oncology, Stanley S. Scott Cancer Center, School of Medicine, Louisiana State University Health Science Center (LSUHSC), 1700 Tulane Avenue, New Orleans, LA, 70012, USA
| | - John H Stewart
- Department of Interdisciplinary Oncology, Stanley S. Scott Cancer Center, School of Medicine, Louisiana State University Health Science Center (LSUHSC), 1700 Tulane Avenue, New Orleans, LA, 70012, USA.
- Louisiana Children's Medical Center Cancer Center, Stanley S. Scott Cancer Center, School of Medicine, Louisiana State University Health Science Center (LSUHSC), 1700 Tulane Avenue, New Orleans, LA, 70012, USA.
- Surgery, Section of Surgical Oncology, Louisiana State University New Orleans-Louisiana Children's Medical Center Cancer Center, Louisiana State University Health Science Center (LSUHSC), 1700 Tulane Avenue, New Orleans, LA, 70012, USA.
| |
Collapse
|
|
35
|
Zhou Z, Guan B, Xia H, Zheng R, Xu B. Particle radiotherapy in the era of radioimmunotherapy. Cancer Lett 2023:216268. [PMID: 37331583 DOI: 10.1016/j.canlet.2023.216268] [Citation(s) in RCA: 3] [Impact Index Per Article: 3.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 03/10/2023] [Revised: 05/24/2023] [Accepted: 06/11/2023] [Indexed: 06/20/2023]
Abstract
Radiotherapy (RT) is one of the key modalities for cancer treatment, and more than 70% of tumor patients will receive RT during the course of their disease. Particle radiotherapy, such as proton radiotherapy, carbon-ion radiotherapy (CIRT) and boron neutron capture therapy (BNCT), is currently available for the treatment of patients Immunotherapy combined with photon RT has been successfully used in the clinic. The effect of immunotherapy combined with particle RT is an area of interest. However, the molecular mechanisms underlying the effects of combined immunotherapy and particle RT remain largely unknown. In this review, we summarize the properties of different types of particle RT and the mechanisms underlying their radiobiological effects. Additionally, we compared the main molecular players in photon RT and particle RT and the mechanisms involved the RT-mediated immune response.
Collapse
Affiliation(s)
- Zihan Zhou
- Department of Radiation Oncology, Fujian Medical University Union Hospital, Xinquan Road 29, Fuzhou, 350000, Fuzhou, China.
| | - Bingjie Guan
- Department of Radiation Oncology, Fujian Medical University Union Hospital, Xinquan Road 29, Fuzhou, 350000, Fuzhou, China.
| | - Huang Xia
- Department of Radiation Oncology, Fujian Medical University Union Hospital, Xinquan Road 29, Fuzhou, 350000, Fuzhou, China.
| | - Rong Zheng
- Department of Radiation Oncology, Fujian Medical University Union Hospital, Xinquan Road 29, Fuzhou, 350000, Fuzhou, China; Fujian Key Laboratory of Intelligent Imaging and Precision Radiotherapy for Tumors (Fujian Medical University), Fuzhou, Xinquan Road 29, Fuzhou, 350000, Fujian, China; Clinical Research Center for Radiology and Radiotherapy of Fujian Province (Digestive, Hematological and Breast Malignancies), Fuzhou, Xinquan Road 29, Fuzhou, 350000, Fujian, China.
| | - Benhua Xu
- Department of Radiation Oncology, Fujian Medical University Union Hospital, Xinquan Road 29, Fuzhou, 350000, Fuzhou, China; Fujian Key Laboratory of Intelligent Imaging and Precision Radiotherapy for Tumors (Fujian Medical University), Fuzhou, Xinquan Road 29, Fuzhou, 350000, Fujian, China; Clinical Research Center for Radiology and Radiotherapy of Fujian Province (Digestive, Hematological and Breast Malignancies), Fuzhou, Xinquan Road 29, Fuzhou, 350000, Fujian, China.
| |
Collapse
|
|
36
|
Tadepalli S, Clements DR, Saravanan S, Hornero RA, Lüdtke A, Blackmore B, Paulo JA, Gottfried-Blackmore A, Seong D, Park S, Chan L, Kopecky BJ, Liu Z, Ginhoux F, Lavine KJ, Murphy JP, Mack M, Graves EE, Idoyaga J. Rapid recruitment and IFN-I-mediated activation of monocytes dictate focal radiotherapy efficacy. Sci Immunol 2023; 8:eadd7446. [PMID: 37294749 PMCID: PMC10340791 DOI: 10.1126/sciimmunol.add7446] [Citation(s) in RCA: 2] [Impact Index Per Article: 2.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 07/01/2022] [Accepted: 05/18/2023] [Indexed: 06/11/2023]
Abstract
The recruitment of monocytes and their differentiation into immunosuppressive cells is associated with the low efficacy of preclinical nonconformal radiotherapy (RT) for tumors. However, nonconformal RT (non-CRT) does not mimic clinical practice, and little is known about the role of monocytes after RT modes used in patients, such as conformal RT (CRT). Here, we investigated the acute immune response induced by after CRT. Contrary to non-CRT approaches, we found that CRT induces a rapid and robust recruitment of monocytes to the tumor that minimally differentiate into tumor-associated macrophages or dendritic cells but instead up-regulate major histocompatibility complex II and costimulatory molecules. We found that these large numbers of infiltrating monocytes are responsible for activating effector polyfunctional CD8+ tumor-infiltrating lymphocytes that reduce tumor burden. Mechanistically, we show that monocyte-derived type I interferon is pivotal in promoting monocyte accumulation and immunostimulatory function in a positive feedback loop. We also demonstrate that monocyte accumulation in the tumor microenvironment is hindered when RT inadvertently affects healthy tissues, as occurs in non-CRT. Our results unravel the immunostimulatory function of monocytes during clinically relevant modes of RT and demonstrate that limiting the exposure of healthy tissues to radiation has a positive therapeutic effect on the overall antitumor immune response.
Collapse
Affiliation(s)
- Sirimuvva Tadepalli
- Department of Microbiology and Immunology, Stanford University School of Medicine, Stanford, CA 94305-5101, USA
- Immunology Program, Stanford University School of Medicine, Stanford, CA 94304, USA
| | - Derek R. Clements
- Department of Microbiology and Immunology, Stanford University School of Medicine, Stanford, CA 94305-5101, USA
- Immunology Program, Stanford University School of Medicine, Stanford, CA 94304, USA
| | - Sanjana Saravanan
- Department of Microbiology and Immunology, Stanford University School of Medicine, Stanford, CA 94305-5101, USA
- Immunology Program, Stanford University School of Medicine, Stanford, CA 94304, USA
| | - Rebeca Arroyo Hornero
- Department of Microbiology and Immunology, Stanford University School of Medicine, Stanford, CA 94305-5101, USA
- Immunology Program, Stanford University School of Medicine, Stanford, CA 94304, USA
| | - Anja Lüdtke
- Department of Microbiology and Immunology, Stanford University School of Medicine, Stanford, CA 94305-5101, USA
- Immunology Program, Stanford University School of Medicine, Stanford, CA 94304, USA
| | - Beau Blackmore
- Department of Biology, University of Prince Edward Island, Charlottetown, PE C1A 4P3, Canada
| | - Joao A. Paulo
- Department of Cell Biology, Harvard Medical School, Boston, MA 02115, USA
| | - Andres Gottfried-Blackmore
- Department of Microbiology and Immunology, Stanford University School of Medicine, Stanford, CA 94305-5101, USA
- Immunology Program, Stanford University School of Medicine, Stanford, CA 94304, USA
- Division of Gastroenterology and Hepatology, Department of Medicine, Stanford University School of Medicine, Redwood City, CA 94063, USA
| | - David Seong
- Department of Microbiology and Immunology, Stanford University School of Medicine, Stanford, CA 94305-5101, USA
- Immunology Program, Stanford University School of Medicine, Stanford, CA 94304, USA
- Medical Scientist Training Program, Stanford University School of Medicine, Stanford, CA 94305-5101, USA
| | - Soyoon Park
- Department of Microbiology and Immunology, Stanford University School of Medicine, Stanford, CA 94305-5101, USA
- Immunology Program, Stanford University School of Medicine, Stanford, CA 94304, USA
| | - Leslie Chan
- Immunology Program, Stanford University School of Medicine, Stanford, CA 94304, USA
| | - Benjamin J. Kopecky
- Center for Cardiovascular Research, Departmental of Medicine, Cardiovascular Division, Washington University School of Medicine, St. Louis, MO 63110, USA
| | - Zhaoyuan Liu
- Shanghai Institute of Immunology, Shanghai Jiao Tong University School of Medicine, Shanghai 200025, China
| | - Florent Ginhoux
- Shanghai Institute of Immunology, Shanghai Jiao Tong University School of Medicine, Shanghai 200025, China
- Institut Gustave Roussy, INSERM U1015, Bâtiment de Médecine Moléculaire, Villejuif 94800, France
- Singapore Immunology Network (SIgN), Agency for Science, Technology and Research (A*STAR), Singapore 138648, Republic of Singapore
| | - Kory J. Lavine
- Center for Cardiovascular Research, Departmental of Medicine, Cardiovascular Division, Washington University School of Medicine, St. Louis, MO 63110, USA
| | - John Patrick Murphy
- Department of Biology, University of Prince Edward Island, Charlottetown, PE C1A 4P3, Canada
| | - Matthias Mack
- Department of Nephrology, University Hospital Regensburg, Regensburg 93053, Germany
| | - Edward E. Graves
- Department of Radiation Oncology, Molecular Imaging Program at Stanford, Stanford University School of Medicine, Stanford, CA 94305-5101, USA
| | - Juliana Idoyaga
- Department of Microbiology and Immunology, Stanford University School of Medicine, Stanford, CA 94305-5101, USA
- Immunology Program, Stanford University School of Medicine, Stanford, CA 94304, USA
| |
Collapse
|
|
37
|
Guo S, Yao Y, Tang Y, Xin Z, Wu D, Ni C, Huang J, Wei Q, Zhang T. Radiation-induced tumor immune microenvironments and potential targets for combination therapy. Signal Transduct Target Ther 2023; 8:205. [PMID: 37208386 DOI: 10.1038/s41392-023-01462-z] [Citation(s) in RCA: 4] [Impact Index Per Article: 4.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 11/30/2022] [Revised: 03/21/2023] [Accepted: 04/27/2023] [Indexed: 05/21/2023] Open
Abstract
As one of the four major means of cancer treatment including surgery, radiotherapy (RT), chemotherapy, immunotherapy, RT can be applied to various cancers as both a radical cancer treatment and an adjuvant treatment before or after surgery. Although RT is an important modality for cancer treatment, the consequential changes caused by RT in the tumor microenvironment (TME) have not yet been fully elucidated. RT-induced damage to cancer cells leads to different outcomes, such as survival, senescence, or death. During RT, alterations in signaling pathways result in changes in the local immune microenvironment. However, some immune cells are immunosuppressive or transform into immunosuppressive phenotypes under specific conditions, leading to the development of radioresistance. Patients who are radioresistant respond poorly to RT and may experience cancer progression. Given that the emergence of radioresistance is inevitable, new radiosensitization treatments are urgently needed. In this review, we discuss the changes in irradiated cancer cells and immune cells in the TME under different RT regimens and describe existing and potential molecules that could be targeted to improve the therapeutic effects of RT. Overall, this review highlights the possibilities of synergistic therapy by building on existing research.
Collapse
Affiliation(s)
- Siyu Guo
- Department of Radiation Oncology, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
- Key Laboratory of Tumor Microenvironment and Immune Therapy of Zhejiang Province, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, National Ministry of Education), Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
- Cancer Center, Zhejiang University, Hangzhou, China
| | - Yihan Yao
- Key Laboratory of Tumor Microenvironment and Immune Therapy of Zhejiang Province, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, National Ministry of Education), Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
| | - Yang Tang
- Key Laboratory of Tumor Microenvironment and Immune Therapy of Zhejiang Province, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, National Ministry of Education), Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
| | - Zengfeng Xin
- Department of Orthopedic Surgery, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
| | - Dang Wu
- Department of Radiation Oncology, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
- Key Laboratory of Tumor Microenvironment and Immune Therapy of Zhejiang Province, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, National Ministry of Education), Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
- Cancer Center, Zhejiang University, Hangzhou, China
| | - Chao Ni
- Key Laboratory of Tumor Microenvironment and Immune Therapy of Zhejiang Province, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, National Ministry of Education), Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
- Cancer Center, Zhejiang University, Hangzhou, China
- Department of Breast Surgery, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
| | - Jian Huang
- Key Laboratory of Tumor Microenvironment and Immune Therapy of Zhejiang Province, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China.
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, National Ministry of Education), Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China.
- Cancer Center, Zhejiang University, Hangzhou, China.
- Department of Breast Surgery, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China.
| | - Qichun Wei
- Department of Radiation Oncology, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China.
- Key Laboratory of Tumor Microenvironment and Immune Therapy of Zhejiang Province, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China.
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, National Ministry of Education), Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China.
| | - Ting Zhang
- Department of Radiation Oncology, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China.
- Key Laboratory of Tumor Microenvironment and Immune Therapy of Zhejiang Province, Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China.
- Cancer Institute (Key Laboratory of Cancer Prevention and Intervention, National Ministry of Education), Second Affiliated Hospital, Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China.
- Cancer Center, Zhejiang University, Hangzhou, China.
| |
Collapse
|
|
38
|
Pan C, Shao S, Gu Y, Ni Q. Radiation prevents tumor progression by inhibiting the miR‑93‑5p/EphA4/NF‑κB pathway in triple‑negative breast cancer. Oncol Rep 2023; 49:78. [PMID: 36866759 DOI: 10.3892/or.2023.8515] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 09/05/2022] [Accepted: 12/28/2022] [Indexed: 03/04/2023] Open
Abstract
Breast cancer (BC) is the most common type of cancer in women. Triple‑negative BC (TNBC) constitutes 10‑15% of all BC cases and is associated with a poor prognosis. It has previously been reported that microRNA (miR)‑93‑5p is dysregulated in plasma exosomes from patients with BC and that miR‑93‑5p improves radiosensitivity in BC cells. The present study identified EphA4 as a potential target gene of miR‑93‑5p and investigated the pathway related to miR‑93‑5p in TNBC. Cell transfection and nude mouse experiments were performed to verify the role of the miR‑93‑5p/EphA4/NF‑κB pathway. Moreover, miR‑93‑5p, EphA4 and NF‑κB were detected in clinical patients. The results revealed that EphA4 and NF‑κB were downregulated in the miR‑93‑5p overexpression group. By contrast, EphA4 and NF‑κB expression levels were not significantly altered in the miR‑93‑5p overexpression + radiation group compared with those in the radiation group. Furthermore, overexpression of miR‑93‑5p with concomitant radiation therapy significantly decreased the growth of TNBC tumors in vivo. In conclusion, the present study revealed that miR‑93‑5p targeted EphA4 in TNBC through the NF‑κB pathway. However, radiation therapy prevented tumor progression by inhibiting the miR‑93‑5p/EphA4/NF‑κB pathway. Therefore, it would be interesting to elucidate the role of miR‑93‑5p in clinical research.
Collapse
|
|
39
|
Fukuda K. Immune Regulation by Cytosolic DNA Sensors in the Tumor Microenvironment. Cancers (Basel) 2023; 15:cancers15072114. [PMID: 37046775 PMCID: PMC10093344 DOI: 10.3390/cancers15072114] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 02/28/2023] [Revised: 03/28/2023] [Accepted: 03/31/2023] [Indexed: 04/05/2023] Open
Abstract
cGAS and AIM2 are CDSs that are activated in the presence of cytosolic dsDNA and are expressed in various cell types, including immune and tumor cells. The recognition of tumor-derived dsDNA by CDSs in the cytosol of tumor-infiltrating dendritic cells (TIDCs) activates the innate and acquired immunity, thereby enhancing anti-tumor immune responses. STING is the downstream signaling effector of cGAS that induces type I interferon (IFN) signaling. Owing to their ability to activate TIDCs, STING agonists have been intratumorally injected in several clinical trials to enhance the anti-tumor immune response elicited by immune checkpoint antibodies. However, they have shown minimal effect, suggesting the importance of optimizing the dose and route of administration for STING agonists and deciphering other immune pathways that contribute to anti-tumor immune responses. Recent studies have revealed that AIM2 activity induces pro-tumor growth through multiple parallel pathways, including inhibition of STING-type I IFN signaling. Thus, AIM2 could be a potential molecular target for cancer immunotherapies. This review summarizes the current research on the roles of cGAS, STING, and AIM2 in immune cells and tumor cells in the tumor microenvironment and discusses the future prospects of anti-tumor treatment approaches based on these molecules.
Collapse
Affiliation(s)
- Keitaro Fukuda
- RIKEN Center for Integrative Medical Sciences (IMS), Laboratory for Skin Homeostasis, Yokohama 230-0045, Japan
- Department of Dermatology, Keio University School of Medicine, Tokyo 160-8582, Japan
| |
Collapse
|
|
40
|
Seo YN, Baik JS, Lee SM, Lee JE, Ahn HR, Lim MS, Park MT, Kim SD. Ionizing Radiation Selectively Increases CXC Ligand 10 Level via the DNA-Damage-Induced p38 MAPK-STAT1 Pathway in Murine J774A.1 Macrophages. Cells 2023; 12:cells12071009. [PMID: 37048082 PMCID: PMC10093567 DOI: 10.3390/cells12071009] [Citation(s) in RCA: 2] [Impact Index Per Article: 2.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/31/2023] [Revised: 03/09/2023] [Accepted: 03/20/2023] [Indexed: 03/29/2023] Open
Abstract
Ionizing radiation (IR) is an important means of tumor treatment in addition to surgery and drugs. Attempts have been made to improve the efficiency of radiotherapy by identifying the various biological effects of IR on cells. Components of the tumor microenvironment, such as macrophages, fibroblasts, and vascular endothelial cells, influence cancer treatment outcomes through communication with tumor cells. In this study, we found that IR selectively increased the production of CXC motif chemokine ligand 10 (CXCL10), which is emerging as an important biomarker for determining the prognosis of anticancer treatments, without changing the levels of CXCL9 and CXCL11 in murine J774A.1 macrophages. Pretreatment with KU55933, an ataxia telangiectasia mutated (ATM) kinase inhibitor, significantly inhibited IR-induced CXCL10 production. In contrast, pretreatment with N-acetyl-cysteine or glutathione, a reactive oxygen species scavenger, did not inhibit IR-induced CXCL10 production. Further, we attempted to identify the intracellular molecular target associated with the IR-induced increase in CXCL10 secretion by J774A.1 macrophages. IR phosphorylated p38 mitogen-activated protein kinase (MAPK) and signal transducer and activator of transcription 1 (STAT1) in J774A.1 macrophages, and p38 MAPK and STAT1 were involved in CXCL10 via IR using pharmacological inhibitors (SB203580 and fludarabine, respectively) and the siRNA technique.
Collapse
Affiliation(s)
- You Na Seo
- Research Center, Dongnam Institute of Radiological & Medical Sciences, Busan 46033, Republic of Korea
- Department of Microbiology and Immunology, College of Medicine, Inge University, Busan 47392, Republic of Korea
| | - Ji Sue Baik
- Research Center, Dongnam Institute of Radiological & Medical Sciences, Busan 46033, Republic of Korea
- Department of Medicinal Biotechnology, College of Health Sciences, Dong-A University, Busan 49315, Republic of Korea
| | - Song Mi Lee
- Department of Veterinary Medicine, College of Veterinary Medicine, Kyoung Pook National University, Daegu 41566, Republic of Korea
| | - Ji Eun Lee
- Department of Veterinary Medicine, College of Veterinary Medicine, Kyoung Pook National University, Daegu 41566, Republic of Korea
| | - Hye Rim Ahn
- Department of Veterinary Medicine, College of Veterinary Medicine, Kyoung Pook National University, Daegu 41566, Republic of Korea
| | - Min Seo Lim
- Department of Veterinary Medicine, College of Veterinary Medicine, Kyoung Pook National University, Daegu 41566, Republic of Korea
| | - Moon-Taek Park
- Research Center, Dongnam Institute of Radiological & Medical Sciences, Busan 46033, Republic of Korea
- Correspondence: (M.-T.P.); (S.D.K.)
| | - Sung Dae Kim
- Department of Veterinary Medicine, College of Veterinary Medicine, Kyoung Pook National University, Daegu 41566, Republic of Korea
- Correspondence: (M.-T.P.); (S.D.K.)
| |
Collapse
|
|
41
|
Kim J, Kim HS, Chung JH. Molecular mechanisms of mitochondrial DNA release and activation of the cGAS-STING pathway. Exp Mol Med 2023; 55:510-519. [PMID: 36964253 PMCID: PMC10037406 DOI: 10.1038/s12276-023-00965-7] [Citation(s) in RCA: 19] [Impact Index Per Article: 19.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 11/20/2022] [Accepted: 12/15/2022] [Indexed: 03/26/2023] Open
Abstract
In addition to constituting the genetic material of an organism, DNA is a tracer for the recognition of foreign pathogens and a trigger of the innate immune system. cGAS functions as a sensor of double-stranded DNA fragments and initiates an immune response via the adaptor protein STING. The cGAS-STING pathway not only defends cells against various DNA-containing pathogens but also modulates many pathological processes caused by the immune response to the ectopic localization of self-DNA, such as cytosolic mitochondrial DNA (mtDNA) and extranuclear chromatin. In addition, macrophages can cause inflammation by forming a class of protein complexes called inflammasomes, and the activation of the NLRP3 inflammasome requires the release of oxidized mtDNA. In innate immunity related to inflammasomes, mtDNA release is mediated by macropores that are formed on the outer membrane of mitochondria via VDAC oligomerization. These macropores are specifically formed in response to mitochondrial stress and tissue damage, and the inhibition of VDAC oligomerization mitigates this inflammatory response. The rapidly expanding area of research on the mechanisms by which mtDNA is released and triggers inflammation has revealed new treatment strategies not only for inflammation but also, surprisingly, for neurodegenerative diseases such as amyotrophic lateral sclerosis.
Collapse
Affiliation(s)
- Jeonghan Kim
- Department of Biochemistry, The Catholic University of Korea College of Medicine, Seoul, 06591, South Korea.
| | - Ho-Shik Kim
- Department of Biochemistry, The Catholic University of Korea College of Medicine, Seoul, 06591, South Korea
| | - Jay H Chung
- Laboratory of Obesity and Aging Research, Cardiovascular Branch, National Heart Lung and Blood Institute, National Institutes of Health, Bethesda, MD, 20892, USA.
| |
Collapse
|
|
42
|
Abstract
Genomic instability is a key driving force for the development and progression of many neurodegenerative diseases and central nervous system (CNS) cancers. The initiation of DNA damage responses is a critical step in maintaining genomic integrity and preventing such diseases. However, the absence of these responses or their inability to repair genomic or mitochondrial DNA damage resulting from insults, including ionizing radiation or oxidative stress, can lead to an accumulation of self-DNA in the cytoplasm. Resident CNS cells, such as astrocytes and microglia, are known to produce critical immune mediators following CNS infection due to the recognition of pathogen and damage-associated molecular patterns by specialized pattern recognition receptors (PRRs). Recently, multiple intracellular PRRs, including cyclic GMP-AMP synthase, interferon gamma-inducible 16, absent in melanoma 2, and Z-DNA binding protein, have been identified as cytosolic DNA sensors and to play critical roles in glial immune responses to infectious agents. Intriguingly, these nucleic acid sensors have recently been shown to recognize endogenous DNA and trigger immune responses in peripheral cell types. In the present review, we discuss the available evidence that cytosolic DNA sensors are expressed by resident CNS cells and can mediate their responses to the presence of self-DNA. Furthermore, we discuss the potential for glial DNA sensor-mediated responses to provide protection against tumorigenesis versus the initiation of potentially detrimental neuroinflammation that could initiate or foster the development of neurodegenerative disorders. Determining the mechanisms that underlie the detection of cytosolic DNA by glia and the relative role of each pathway in the context of specific CNS disorders and their stages may prove pivotal in our understanding of the pathogenesis of such conditions and might be leveraged to develop new treatment modalities.
Collapse
Affiliation(s)
| | - Ian Marriott
- Department of Biological Sciences, University of North Carolina at Charlotte, Charlotte, NC, United States
| |
Collapse
|
|
43
|
Beernaert B, Parkes EE. cGAS-STING signalling in cancer: striking a balance with chromosomal instability. Biochem Soc Trans 2023:BST20220838. [PMID: 36876871 DOI: 10.1042/BST20220838] [Citation(s) in RCA: 9] [Impact Index Per Article: 9.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 11/14/2022] [Revised: 01/19/2023] [Accepted: 01/23/2023] [Indexed: 03/07/2023]
Abstract
Chromosomal instability (CIN) is a hallmark of cancer that drives tumour evolution. It is now recognised that CIN in cancer leads to the constitutive production of misplaced DNA in the form of micronuclei and chromatin bridges. These structures are detected by the nucleic acid sensor cGAS, leading to the production of the second messenger 2'3'-cGAMP and activation of the critical hub of innate immune signalling STING. Activation of this immune pathway should instigate the influx and activation of immune cells, resulting in the eradication of cancer cells. That this does not universally occur in the context of CIN remains an unanswered paradox in cancer. Instead, CIN-high cancers are notably adept at immune evasion and are highly metastatic with typically poor outcomes. In this review, we discuss the diverse facets of the cGAS-STING signalling pathway, including emerging roles in homeostatic processes and their intersection with genome stability regulation, its role as a driver of chronic pro-tumour inflammation, and crosstalk with the tumour microenvironment, which may collectively underlie its apparent maintenance in cancers. A better understanding of the mechanisms whereby this immune surveillance pathway is commandeered by chromosomally unstable cancers is critical to the identification of new vulnerabilities for therapeutic exploitation.
Collapse
|
|
44
|
Feng DC, Zhu WZ, Shi X, Xiong Q, You J, Wei Q, Yang L. Identification of senescence-related molecular subtypes and key genes for prostate cancer. Asian J Androl 2023; 25:223-229. [PMID: 36124532 PMCID: PMC10069687 DOI: 10.4103/aja202258] [Citation(s) in RCA: 8] [Impact Index Per Article: 8.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Indexed: 11/04/2022] Open
Abstract
We identified distinct senescence-related molecular subtypes and critical genes among prostate cancer (PCa) patients undergoing radical prostatectomy (RP) or radical radiotherapy (RT). We conducted all analyses using R software and its suitable packages. Twelve genes, namely, secreted frizzled-related protein 4 (SFRP4), DNA topoisomerase II alpha (TOP2A), pleiotrophin (PTN), family with sequence similarity 107 member A (FAM107A), C-X-C motif chemokine ligand 14 (CXCL14), prostate androgen-regulated mucin-like protein 1 (PARM1), leucine zipper protein 2 (LUZP2), cluster of differentiation 38 (CD38), cartilage oligomeric matrix protein (COMP), vestigial-like family member 3 (VGLL3), apolipoprotein E (APOE), and aldehyde dehydrogenase 2 family member (ALDH2), were eventually used to subtype PCa patients from The Cancer Genome Atlas (TCGA) database and GSE116918, and the molecular subtypes showed good correlations with clinical features. In terms of the tumor immune environment (TME) analysis, compared with cluster 1, cancer-associated fibroblasts (CAFs) scored significantly higher, while endothelial cells scored lower in cluster 2 in TCGA database. There was a statistically significant correlation between both CAFs and endothelial cells with biochemical recurrence (BCR)-free survival for PCa patients undergoing RP. For the GSE116918 database, cluster 2 had significantly lower levels of CAFs and tumor purity and higher levels of stromal, immune, and Estimation of STromal and Immune cells in MAlignant Tumor tissues using Expression data (ESTIMATE) scores than cluster 1; in addition, patients with high levels of CAFs, stromal scores, immune scores, and ESTIMATE scores and low levels of tumor purity tended to suffer from BCR. Based on the median of differentially expressed checkpoints, high expression of CD96, hepatitis A virus cellular receptor 2 (HAVCR2), and neuropilin 1 (NRP1) in GSE116918 and high expression of CD160 and tumor necrosis factor (ligand) superfamily member 18 (TNFSF18) in TCGA database were associated with a significantly higher risk of BCR than their counterparts. In conclusion, we first constructed distinct molecular subtypes and critical genes for PCa patients undergoing RP or RT from the fresh perspective of senescence.
Collapse
Affiliation(s)
- De-Chao Feng
- Department of Urology, Institute of Urology, West China Hospital, Sichuan University, Chengdu 610041, China
| | - Wei-Zhen Zhu
- Department of Urology, Institute of Urology, West China Hospital, Sichuan University, Chengdu 610041, China
| | - Xu Shi
- Department of Urology, Institute of Urology, West China Hospital, Sichuan University, Chengdu 610041, China
| | - Qiao Xiong
- Department of Urology, Institute of Urology, West China Hospital, Sichuan University, Chengdu 610041, China
| | - Jia You
- Department of Urology, Institute of Urology, West China Hospital, Sichuan University, Chengdu 610041, China
| | - Qiang Wei
- Department of Urology, Institute of Urology, West China Hospital, Sichuan University, Chengdu 610041, China
| | - Lu Yang
- Department of Urology, Institute of Urology, West China Hospital, Sichuan University, Chengdu 610041, China
| |
Collapse
|
|
45
|
Zhang X, Zhang H, Zhang J, Yang M, Zhu M, Yin Y, Fan X, Yu F. The paradoxical role of radiation-induced cGAS-STING signalling network in tumour immunity. Immunology 2023; 168:375-388. [PMID: 36217274 DOI: 10.1111/imm.13592] [Citation(s) in RCA: 2] [Impact Index Per Article: 2.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 05/28/2022] [Accepted: 10/06/2022] [Indexed: 11/27/2022] Open
Abstract
The cyclic GMP-AMP synthase-stimulator of interferon genes (cGAS-STING) pathway is an essential component of the innate immune system and is central to the identification of abnormal DNA leakage caused by ionising radiation (IR) damage. Cell-intrinsic cGAS-STING initiation has been revealed to have tremendous potential for facilitating interferon synthesis and T-cell priming. Targeting the cGAS-STING axis has been proposed as a strategy to improve radiosensitivity or enhance immunosurveillance. However, due to the complex biology of the irradiated tumour microenvironment and the extensive involvement of the cGAS-STING pathway in various physiological and pathological processes, many defects in this strategy limit the therapeutic effect. Here, we outline the molecular mechanisms by which IR activates the cGAS-STING pathway and analyse the dichotomous roles of the cGAS-STING pathway in modulating cancer immunity after radiotherapy (RT). Then, based on the crosstalk between the cGAS-STING pathway and other signalling events induced by IR, such as necroptosis, autophagy and other cellular effects, we discuss the immunomodulatory actions of the broad cGAS-STING signalling network in RT and their potential therapeutic applications. Finally, recent advances in combination therapeutic strategies targeting cGAS-STING in RT are explored.
Collapse
Affiliation(s)
- Xiaoyi Zhang
- Department of Nuclear Medicine, Shanghai Tenth People's Hospital, Tongji University School of Medicine, Shanghai, China.,Institute of Nuclear Medicine, Tongji University School of Medicine, Shanghai, China
| | - Han Zhang
- Department of Nuclear Medicine, Shanghai Tenth People's Hospital, Tongji University School of Medicine, Shanghai, China.,Institute of Nuclear Medicine, Tongji University School of Medicine, Shanghai, China
| | - Jiajia Zhang
- Department of Nuclear Medicine, Shanghai Tenth People's Hospital, Tongji University School of Medicine, Shanghai, China.,Institute of Nuclear Medicine, Tongji University School of Medicine, Shanghai, China
| | - Mengdie Yang
- Department of Nuclear Medicine, Shanghai Tenth People's Hospital, Tongji University School of Medicine, Shanghai, China.,Institute of Nuclear Medicine, Tongji University School of Medicine, Shanghai, China
| | - Mengqin Zhu
- Department of Nuclear Medicine, Shanghai Tenth People's Hospital, Tongji University School of Medicine, Shanghai, China.,Institute of Nuclear Medicine, Tongji University School of Medicine, Shanghai, China
| | - Yuzhen Yin
- Department of Nuclear Medicine, Shanghai Tenth People's Hospital, Tongji University School of Medicine, Shanghai, China.,Institute of Nuclear Medicine, Tongji University School of Medicine, Shanghai, China
| | - Xin Fan
- Department of Nuclear Medicine, Shanghai Tenth People's Hospital, Tongji University School of Medicine, Shanghai, China.,Institute of Nuclear Medicine, Tongji University School of Medicine, Shanghai, China
| | - Fei Yu
- Department of Nuclear Medicine, Shanghai Tenth People's Hospital, Tongji University School of Medicine, Shanghai, China.,Institute of Nuclear Medicine, Tongji University School of Medicine, Shanghai, China
| |
Collapse
|
|
46
|
Li K, Qin Y, Ye L. Response to 'Hyperbaric oxygen facilitates teniposide-induced cGAS-STING activation to enhance the antitumor efficacy of PD-1 antibody in HCC' by Yang et al. J Immunother Cancer 2023; 11:jitc-2022-006648. [PMID: 36882227 PMCID: PMC10008227 DOI: 10.1136/jitc-2022-006648] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Accepted: 02/21/2023] [Indexed: 03/09/2023] Open
Affiliation(s)
- Kun Li
- Department of Hepatic Surgery and Liver Transplantation Center, Third Affiliated Hospital of Sun Yat-Sen University, Guangzhou, Guangdong, China
| | - Yunfei Qin
- Department of Biotherapy Center, Third Affiliated Hospital of Sun Yat-Sen University, Guangzhou, Guangdong, China
| | - Linsen Ye
- Department of Hepatic Surgery and Liver Transplantation Center, Third Affiliated Hospital of Sun Yat-Sen University, Guangzhou, Guangdong, China
| |
Collapse
|
|
47
|
Zhang L, Wei X, Wang Z, Liu P, Hou Y, Xu Y, Su H, Koci MD, Yin H, Zhang C. NF-κB activation enhances STING signaling by altering microtubule-mediated STING trafficking. Cell Rep 2023; 42:112185. [PMID: 36857187 DOI: 10.1016/j.celrep.2023.112185] [Citation(s) in RCA: 25] [Impact Index Per Article: 25.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 09/09/2022] [Revised: 01/12/2023] [Accepted: 02/14/2023] [Indexed: 03/02/2023] Open
Abstract
It is widely known that stimulator of interferon genes (STING) can trigger nuclear factor κB (NF-κB) signaling. However, whether and how the NF-κB pathway affects STING signaling remains largely unclear. Here, we report that Toll-like receptor (TLR)-, interleukin-1 receptor (IL-1R)-, tumor necrosis factor receptor (TNFR)-, growth factor receptor (GF-R)-, and protein kinase C (PKC)-mediated NF-κB signaling activation dramatically enhances STING-mediated immune responses. Mechanistically, we find that STING interacts with microtubules, which plays a crucial role in STING intracellular trafficking. We further uncover that activation of the canonical NF-κB pathway induces microtubule depolymerization, which inhibits STING trafficking to lysosomes for degradation. This leads to increased levels of activated STING that persist for a longer period of time. The synergy between NF-κB and STING triggers a cascade-amplified interferon response and robust host antiviral defense. In addition, we observe that several gain-of-function mutations of STING abolish the microtubule-STING interaction and cause abnormal STING trafficking and ligand-independent STING autoactivation. Collectively, our data demonstrate that NF-κB activation enhances STING signaling by regulating microtubule-mediated STING trafficking.
Collapse
Affiliation(s)
- Lulu Zhang
- School of Pharmaceutical Sciences, Tsinghua University, Beijing 100084, China; Tsinghua-Peking Center for Life Sciences, Beijing 100084, China
| | - Xubiao Wei
- School of Pharmaceutical Sciences, Tsinghua University, Beijing 100084, China; Tsinghua-Peking Center for Life Sciences, Beijing 100084, China
| | - Zhimeng Wang
- School of Pharmaceutical Sciences, Tsinghua University, Beijing 100084, China; Tsinghua-Peking Center for Life Sciences, Beijing 100084, China
| | - Peiyuan Liu
- School of Life Science, Tianjin University, Tianjin, China
| | - Yanfei Hou
- School of Pharmaceutical Sciences, Tsinghua University, Beijing 100084, China
| | - Yifang Xu
- School of Pharmaceutical Sciences, Tsinghua University, Beijing 100084, China
| | - Huili Su
- School of Pharmaceutical Sciences, Tsinghua University, Beijing 100084, China
| | - Matthew D Koci
- Prestage Department of Poultry Science, College of Agriculture and Life Sciences, North Carolina State University, Raleigh, NC, USA
| | - Hang Yin
- School of Pharmaceutical Sciences, Tsinghua University, Beijing 100084, China; Tsinghua-Peking Center for Life Sciences, Beijing 100084, China.
| | - Conggang Zhang
- School of Pharmaceutical Sciences, Tsinghua University, Beijing 100084, China; Tsinghua-Peking Center for Life Sciences, Beijing 100084, China.
| |
Collapse
|
|
48
|
Long Y, Guo J, Chen J, Sun J, Wang H, Peng X, Wang Z, Lai W, Liu N, Shu L, Chen L, Shi Y, Xiao D, Liu S, Tao Y. GPR162 activates STING dependent DNA damage pathway as a novel tumor suppressor and radiation sensitizer. Signal Transduct Target Ther 2023; 8:48. [PMID: 36725837 DOI: 10.1038/s41392-022-01224-3] [Citation(s) in RCA: 7] [Impact Index Per Article: 7.0] [Reference Citation Analysis] [What about the content of this article? (0)] [Abstract] [Key Words] [Track Full Text] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 02/10/2022] [Revised: 09/05/2022] [Accepted: 10/09/2022] [Indexed: 02/03/2023] Open
Abstract
In the treatment of most malignancies, radiotherapy plays a significant role. However, the resistance of cancer cells to ionizing radiation (IR) is the main reason for the failure of radiotherapy, which causes tumor recurrence and metastasis. In this study, we confirmed that GPR162, an orphan receptor in the G-protein-coupled receptor family, acted as a novel radiotherapy sensitizer by interacting with the stimulator of interferon genes (STING), which targeted DNA damage responses, activated IRF3, accelerated the activation of type I interferon system, promoted the expression of chemokines including CXCL10 and CXCL4, and inhibited the occurrence and development of tumors. Interestingly, the activation of STING by overexpression of GPR162 was independent of the classical pathway of cGAS. STING inhibitors could resist the antitumor effect of overexpression of GPR162 in IR-induced mouse models. In addition, most solid tumors showed low expression of GPR162. And the higher expression of GPR162 indicated a better prognosis in patients with lung adenocarcinoma, liver cancer, breast cancer, etc. In summary, these results suggested that GPR162 may serve as a potential sensitizer of radiotherapy by promoting radiotherapy-induced STING-IFN production and increasing the expression of chemokines including CXCL10 and CXCL4 in DNA damage response, providing an alternative strategy for improving cancer radiotherapy.
Collapse
|
|
49
|
Wang XY, Beeraka NM, Xue NN, Yu HM, Yang Y, Liu MX, Nikolenko VN, Liu JQ, Zhao D. Identification of a three-gene prognostic signature for radioresistant esophageal squamous cell carcinoma. World J Clin Oncol 2023; 14:13-26. [PMID: 36699628 PMCID: PMC9850665 DOI: 10.5306/wjco.v14.i1.13] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Journal Information] [Submit a Manuscript] [Subscribe] [Scholar Register] [Received: 07/25/2022] [Revised: 10/25/2022] [Accepted: 12/06/2022] [Indexed: 01/10/2023] Open
Abstract
BACKGROUND Esophageal squamous cell carcinoma (ESCC) is causing a high mortality rate due to the lack of efficient early prognosis markers and suitable therapeutic regimens. The prognostic role of genes responsible for the acquisition of radioresistance in ESCC has not been fully elucidated.
AIM To establish a prognostic model by studying gene expression patterns pertinent to radioresistance in ESCC patients.
METHODS Datasets were obtained from the Gene Expression Omnibus and The Cancer Genome Atlas databases. The edgeR, a Bioconductor package, was used to analyze mRNA expression between different groups. We screened genes specifically responsible for radioresistance to estimate overall survival. Pearson correlation analysis was performed to confirm whether the expression of those genes correlated with each other. Genes contributing to radioresistance and overall survival were assessed by the multivariate Cox regression model through the calculation of βi and risk score using the following formula: 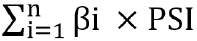 . .
RESULTS We identified three prognostic mRNAs (cathepsin S [CTSS], cluster of differentiation 180 [CD180], and SLP adapter and CSK-interacting membrane protein [SCIMP]) indicative of radioresistance. The expression of the three identified mRNAs was related to each other (r > 0.70 and P < 0.05). As to 1-year and 3-year overall survival prediction, the area under the time-dependent receiver operating characteristic curve of the signature consisting of the three mRNAs was 0.716 and 0.841, respectively. When stratifying patients based on the risk score derived from the signature, the high-risk group exhibited a higher death risk and shorter survival time than the low-risk group (P < 0.0001). Overall survival of the low-risk patients was significantly better than that of the high-risk patients (P = 0.018).
CONCLUSION We have developed a novel three-gene prognostic signature consisting of CTSS, CD180, and SCIMO for ESCC, which may facilitate the prediction of early prognosis of this malignancy.
Collapse
Affiliation(s)
- Xiao-Yan Wang
- Department of Endocrinology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou 450052, Henan Province, China
| | - Narasimha M Beeraka
- Department of Radiation Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou 450052, Henan Province, China
- Department of Human Anatomy, I. M. Sechenov First Moscow State Medical University, Moscow 119991, Russia
- Department of Pharmaceutical Chemistry, JSS College of Pharmacy, Mysuru 570015, India
| | - Nan-Nan Xue
- Department of Radiation Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou 450052, Henan Province, China
| | - Hui-Ming Yu
- Department of Radiation Oncology, Peking University Cancer Hospital & Institute, Beijing 065005, China
| | - Ya Yang
- Department of Radiation Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou 450052, Henan Province, China
| | - Mao-Xing Liu
- Key Laboratory of Carcinogenesis and Translational Research (Ministry of Education), Department of Gastrointestinal Surgery IV, Peking University Cancer Hospital & Institute, Beijing, China
| | - Vladimir N Nikolenko
- Department of Human Anatomy, I. M. Sechenov First Moscow State Medical University, Moscow 119991, Russia
- M.V. Lomonosov Moscow State University, Moscow 119991, Russia
| | - Jun-Qi Liu
- Department of Radiation Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou 450052, Henan Province, China
| | - Di Zhao
- Department of Endocrinology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou 450052, Henan Province, China
| |
Collapse
|
|
50
|
Brouiller F, Nadalin F, Bonté PE, Ait-Mohamed O, Delaugerre C, Lelièvre JD, Ginhoux F, Ruffin N, Benaroch P. Single-cell RNA-seq analysis reveals dual sensing of HIV-1 in blood Axl + dendritic cells. iScience 2023; 26:106019. [PMID: 36866043 PMCID: PMC9971904 DOI: 10.1016/j.isci.2023.106019] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [What about the content of this article? (0)] [Affiliation(s)] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 06/15/2022] [Revised: 11/05/2022] [Accepted: 01/17/2023] [Indexed: 01/22/2023] Open
Abstract
Sensing of incoming viruses is a pivotal task of dendritic cells (DCs). Human primary blood DCs encompass various subsets that are diverse in their susceptibility and response to HIV-1. The recent identification of the blood Axl+DC subset, endowed with unique capacities to bind, replicate, and transmit HIV-1 prompted us to evaluate its anti-viral response. We demonstrate that HIV-1 induced two main broad and intense transcriptional programs in different Axl+DCs potentially induced by different sensors; an NF-κB-mediated program that led to DC maturation and efficient CD4+ T cell activation, and a program mediated by STAT1/2 that activated type I IFN and ISG responses. These responses were absent from cDC2 exposed to HIV-1 except when viral replication was allowed. Finally, Axl+DCs actively replicating HIV-1 identified by quantification of viral transcripts exhibited a mixed NF-κB/ISG innate response. Our results suggest that the route of HIV-1 entry may dictate different innate sensing pathways by DCs.
Collapse
Affiliation(s)
- Flavien Brouiller
- Institut Curie, PSL∗ Research University, INSERM U 932, 75005 Paris, France
| | - Francesca Nadalin
- Institut Curie, PSL∗ Research University, INSERM U 932, 75005 Paris, France
| | | | | | - Constance Delaugerre
- Laboratoire de Virologie, Hôpital Saint Louis, Assistance Publique-Hôpitaux de Paris, Paris, France,INSERM U944, Université de Paris, Paris, France
| | - Jean-Daniel Lelièvre
- Vaccine Research Institute, Institut National de la Santé et de la Recherche médicale (INSERM), Assistance Publique Hôpitaux de Paris (APHP), Hôpital H. Mondor, Créteil, France
| | - Florent Ginhoux
- Singapore Immunology Network (SIgN), A∗STAR, 8A Biomedical Grove, Immunos Building, Level 4, Singapore 138648, Singapore,Shanghai Institute of Immunology, Department of Immunology and Microbiology, Shanghai Jiao Tong University School of Medicine, Shanghai 200025, China,Translational Immunology Institute, SingHealth Duke-NUS Academic Medical Centre, Singapore 169856, Singapore
| | - Nicolas Ruffin
- Institut Curie, PSL∗ Research University, INSERM U 932, 75005 Paris, France,Corresponding author
| | - Philippe Benaroch
- Institut Curie, PSL∗ Research University, INSERM U 932, 75005 Paris, France,Corresponding author
| |
Collapse
|